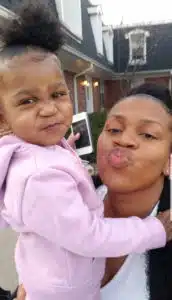Our Patients:
Aaryn Wiley

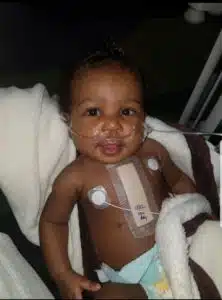
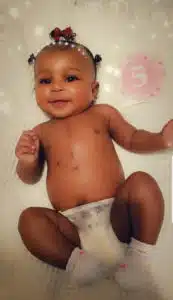
Watching sassy two-year-old Aaryn have a meltdown, or dancing and singing to her favorite cartoons, one would never guess that she had a much more fragile start to life. For Mom Hannah – watching this “normal” child behavior is a gift she wasn’t sure she’d ever get.
Hannah was working in 2017 as a full-time postal worker. She is the 3rd of 8 children in her own family, and always longed of being a mom, herself. After several years of not conceiving, she had all but given up. “I remember going Christmas shopping that year in November and feeling extra sluggish and tired. My friend encouraged me to take a pregnancy test, and I was shocked to learn that I was pregnant!” Hannah said.
As many pregnant moms do, Hannah envisioned what life would be like with her new baby, and she anxiously awaited the gender ultrasound appointment. She went to that appointment at SSM Health St. Mary’s Hospital, and was told by the Ultrasound technician that she was having a girl. Hannah was elated and patient for the next hour of her scan. But that hour turned into another hour, and then another hour. “I actually fell asleep because it was taking so long,” Hannah said, “When I looked at the time, it had been over 3 hours. I hadn’t been too concerned because I had never had an ultrasound before. No one was with me, and it was my first pregnancy, so I didn’t really think anything of it, until I saw more people coming in the room,” Hannah said. “I remember the tech saying that she couldn’t find my baby’s heart. She sent in another nurse, and then she brought in the doctor. Hannah recalled what the doctor said as he reviewed and stared at the ultrasound. He said, “Your baby’s heart isn’t developing normally, he said. I want you to go see Dr. Reddy at Cardinal Glennon.”
Hannah immediately began grieving the loss of her “perfect baby” and wondering how this could have happened. “I prayed and I prayed. I called my mom, and I prayed some more. I hoped when I went to see this Dr. Reddy that she would tell me everything was fine,” Hannah said.
Three days later, Hannah visited the St. Louis Fetal Care Institute at SSM Health Cardinal Glennon Children’s Hospital. She met Pediatric Cardiologist, Dr. Chetana Reddy, and SLUCare Cardiothoracic Surgeon, Dr. Charles Huddleston. Her ultrasound confirmed what the other had suggested – that baby Aaryn’s heart was NOT developing normally. Hannah appreciated that Dr. Reddy did her own ultrasound. It helped to reinforce to her that there had not been a “mistake”. Dr. Huddleston suspected that Aaryn had a condition called Truncus Arteriosus, but only time would confirm the specific defect for sure.
Truncus arteriosus is a rare defect of the heart in which a single common blood vessel comes out of the heart, instead of the usual two vessels (the main pulmonary artery and aorta). In babies with a truncus arteriosus, oxygen-poor blood and oxygen-rich blood are mixed together as blood flows to the lungs and the rest of the body. As a result, too much blood goes to the lungs and the heart works harder to pump blood to the rest of the body. Truncus arteriosus occurs in less than one out of every 10,000 live births. There are about 250 cases of truncus arteriosus per year in the United States.
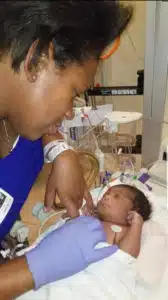
“I saw Dr. Reddy about every two weeks until I delivered. At my last prenatal visit with my OB, they told me I had pre-eclampsia. They kept me to begin induction right away, and I was in labor for 3 ½ days. I ended up having an emergency C-section on August 5th , and they took Aaryn right away to Cardinal Glennon. Since I had a C-section and had so many drugs on board, I didn’t even get to say goodbye to her, “ Hannah said.
For babies with truncus arteriosus, surgery is needed to repair the heart and blood vessels. This is usually done in the first few months of life. During her prenatal visits to the St. Louis Fetal Care Institute, Hannah was prepared for Aaryn to have surgery immediately after birth.
Options for repair depend on how sick the child is and the specific structure of the defect. The goal of the surgery is to create a separate flow of oxygen-poor blood to the lungs and oxygen-rich blood to the body.
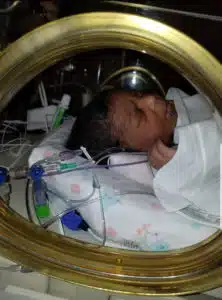
As it turns out, Aaryn’s vessels and arteries were smaller and narrower than what was ideal for surgery. She was also maintaining her breathing independently without the need for intubation and ventilator support. The decision was made to “watch and wait” and let her little body grow as much as possible before her first surgery. Aaryn remained in the hospital for 29 days, and was discharged home with a plan to monitor and follow her carefully. At the same time Aaryn was in the NICU. Hannah admittedly was dealing with some post-partum depression. “I couldn’t see my baby for the first 8 days, since I was recovering from a C-section. Between the separation, not being able to hold her, not being able to feed her, and worrying about her condition, I lost a lot of weight, I wasn’t eating, and I was having trouble bonding, “admits Hannah. “After we went home, I felt like I was calling constantly. We were back and forth to the hospital every 2-3 weeks to check in,” Hannah said, “but I was definitely glad to be home.”
Throughout the months of November and December 2018, Aaryn was showing increased signs of poor oxygen flow. Her oxygen saturation monitor numbers worsened. She grew tired more easily, and her skin was more “purplish” in color. With a watchful eye, the team decided to wait until after the holidays, but to plan Aaryn’s surgery for early January. The goal of Aaryn’s first surgery would be to create a separate flow of oxygen-poor blood to the lungs and oxygen-rich blood to the body. Usually, surgery to repair this defect involves closing the hole between the bottom chambers of the heart with a patch; using the original single blood vessel to create a new aorta to carry oxygen-rich blood from the left ventricle out to the body; and using an artificial tube (conduit) with an artificial valve to connect the right ventricle to the arteries going to the lungs in order to carry oxygen-poor blood to the lungs.
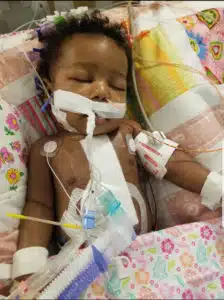
“I went to church on January 6th,” Hannah said. “The whole church said prayers for my baby’s successful surgery. The next day came so fast, and it seemed like she was in surgery forever, “ said Hannah. “ “As I was waiting for Aaryn to get out of surgery, I found out on Facebook that my Auntie had passed away. I figured no one had called me, so as not to worry about anything besides my own baby – but it just made everything worse – especially when I saw the nurse come into the waiting room to talk to me. I asked the nurse if Aaryn’s surgery was over, and she said, ‘no’, that they had to put my baby on life support. She told me they had a scare and that there was too much swelling to close her chest. They temporarily had her on life support for proper blood flow, with her heart outside her chest,” Hannah said. “I completely panicked and ran out of the waiting room crying, heading straight to the chapel. Looking back on it now, I didn’t know what she really meant. I just heard the words ‘life support’ and thought this might be the end, “ said Hannah.
Hannah recalls Aaryn’s father helping her out of the chapel and back to the Pediatric Intensive Care Unit. The surgeons were able to finish Aaryn’s surgery successfully, and close her chest before taking her to the PICU. “There were so many tubes and machines. I could only look at her for a minute before needing to get some fresh air. It’s a hard environment there. Another baby in a room not too far from us died, and all I could think of is if that would happen to Aaryn. I feel like I prayed non-stop for days. But days passed, Aaryn kept getting better, and machines and medications were eventually weaned off,” Hannah said.
Aaryn was discharged after a 2 week hospital stay. Hannah brought her back to the Dorothy and Larry Dallas Heart Center to see Dr. Reddy almost every 2 weeks for check-ups. Aaryn was also being followed by First Steps in an effort to make sure she was reaching her developmental milestones.
At age 1, Aaryn began having lower oxygen levels again. Most babies with truncus arteriosus survive the initial surgical repair, but may need more surgery or other procedures as they get older. For example, the artificial tube doesn’t grow, so it will need to be replaced as the child grows. Some babies with truncus arteriosus will need medicines to help strengthen the heart muscle, lower their blood pressure, or help their body get rid of extra fluid. Dr. Reddy tried different medications with Aaryn. If they could avoid another surgery soon, that is what they wanted to do.
In July 2020, Aaryn had a second surgery. “We couldn’t manage her symptoms with just medication anymore, so we had to do the surgery. She didn’t really have any significant complications, though, so that was a blessing,” Hannah says. “She’ll probably need at least two more surgeries in her future, because her conduit needs to grow as SHE grows. The conduit is also an artificial device, so if any infection gets to it, it has to be taken out,” she says. “I’m a real stickler when it comes to cleaning! Bleach is a wonderful thing,” Hannah laughs. “When the pandemic came, we were already used to cleaning and extra protection measures. We did it all the time, already,” emphasizes Hannah.
When asked about the Dorothy and Larry Dallas Heart Center, Hannah states, “It’s the place you never wanted to have a family, that’s like a family!” “Everyone knows my baby, and everyone is so compassionate and loving – from the doctors to the nurses to the receptionist to her echo techs – EVERYONE,” she says. Hannah and Dr. Reddy, especially, have shared a special bond. “She told me when I was still pregnant that she was going to take care of me, and she also told me that I had to trust her. She gave me her word, and she gave me pointers and a plan for what was going to happen. I was so scared, and she was upfront. Dr. Reddy’s my girl, and I respect her,” Hannah says.
“Dr. Reddy, Dr. Huddleston, and everyone at the Dallas Heart Center, have given Aaryn and I a chance at chance at a good future. I try not to treat her like a heart patient. I am mindful of her limits, but I want her to do anything her body allows her. I want to go to her track meets, watch her do gymnastics, and be the loud, obnoxious mom in the stands cheering her on,” Hannah laughs. “She will definitely be making school and health her priorities. When she’s successful, I look forward to being the mom who can remind her where she started, and give her the confidence to do anything she wants.”