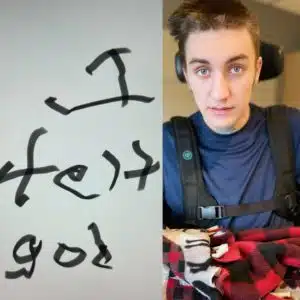Our Patients:
Colton Friese

On October 16, 2020, at approximately 4:30pm, 19 year-old Colton was on his way home from work driving his reliable Chevy Cobalt. He had proudly saved and bought himself a Dodge Charger in March 2020 before the pandemic started, but he liked saving his “pride and joy” for special occasions vs. day-to-day travel. Colton was a full time freshman student in the Pre-Dental program at Southeast Missouri State, and he worked part time helping to build houses at J&J Construction in his hometown of Jackson, MO. That 16th day of October, at a very familiar intersection, Colton stopped in advance of making a turn. Before he knew it, another car approaching the intersection slammed on their brakes, clipping his car and placing him in the middle of traffic. A truck with a camper hit Colton’s car head-on, and witnessed called 911 to the scene. One of the first responders would later tell Colton’s mother, Tonya, in a letter, that “rescuing Colton from his car was one of the fastest extractions he had ever been part of”. Colton was extracted within 5 minutes of EMS arrival to the scene and was immediately transported via ambulance to the closest local hospital – St. Francis Hospital in Jackson, MO.
A friend of Colton’s family drove by the accident scene and recognized Colton’s car. He called Tonya and asked, “Has Colton been in an accident?” Shocked, and realizing that Colton should have arrived home from work by that point, Tonya immediately attempted to track Colton’s phone. The tracker showed Colton’s phone moving in the opposite direction of home, causing alarm and suspicion that something wasn’t right. Tonya’s next step was calling St. Francis Hospital. No one could have prepared her for what she was told next.
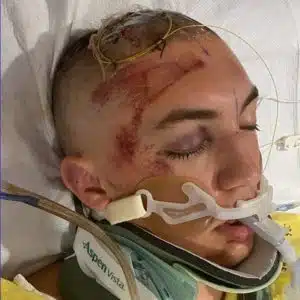
Tonya was told that an “unidentified teenage male, trauma victim, car accident”, had just been brought in via ambulance with no ID. Living approximately 30 minutes from the hospital, Tonya and her husband immediately headed there, devastated and frightened that this young man could be their son. Upon arrival to the hospital, they immediately identified Colton, and an incomprehensible scenario was unfolding all around them. Colton went into cardiac arrest while Tonya and Dylan were still in the room. He had several open fractures to his arms and legs, damage to multiple internal organs, and profound blood loss. It was determined quickly at St. Francis that Colton needed the trauma care and expertise available at SSM Health St. Louis University Hospital in St. Louis. The first and most immediate goal was stabilizing him for transport. The team at St. Francis prepared Colton’s family for the extreme likelihood that he might not survive the helicopter ride to SLU.
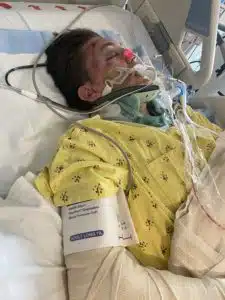
Colton arrived to SLU alive and he had his first of multiple surgeries that evening at 11:45pm. His spleen was removed. His diaphragm was repaired. He received 27 units of blood. All of his ribs were broken and he had several broken bones. Those were on a list of many things that would need to be addressed in subsequent surgeries. Over the next couple weeks, he had surgery on his right arm, surgery on his right hand, surgeries on both legs, surgery on his pelvis. He had a plate and screws placed in his right arm, a rod placed from his right hip to right knee, a rod placed from his left knee to left ankle, a plate and screws placed in his right arm, and pins and screws placed in his right hand. His pelvis and leg were completely severed in half requiring a plate and screws to his hip. Ten days following that long chain of surgeries, Colton had a tracheostomy placed and a feeding tube placed in his stomach.
Despite the fact that Colton was alive, and surgeries were successfully addressing many of his complex injuries, Colton had additional complications that were challenging at best. He suffered from high fevers, from brain bleeds, and “neuro-storming”. “Storming” is a term to describe an onset of symptoms that can sometimes happen following a traumatic brain injury. Symptoms can include alterations in consciousness, involuntary muscle movements, fevers, high blood pressure, rapid heart rate, rapid breathing, sweating and agitation. Many times following a traumatic brain injury, patients who experience “neuro storming” are at a low level of neurological activity with minimal alertness, minimal awareness, and reflexive motor response to stimulation, and the storming can take a seemingly peaceful individual into a state of chaos. Treatment is aimed at controlling the duration and severity of the symptoms and preventing additional brain injury. Colton was also found to have an E-Coli infection in his lungs and his bloodstream, and his fevers persisted for weeks.
“Throughout his healing period at SLU, Colton never seemed to really wake up,” recalled Tonya. “We really weren’t seeing progress, and his team wasn’t sure that we could every expect to see a change in his mental status,” Tonya said. “As the weeks went on, the plans discussed were to either send him home in this state, or send him to a nursing home,” Tonya said. “I don’t think anyone anticipated that Colton was destined for anything more than he was presenting at the time,” she said.
“To make matters worse, we were restricted from visiting him because of COVID visitation guidelines. So when I say we weren’t seeing progress – we truly weren’t because we weren’t able to lay eyes on him. We relied on over-the phone reports from his caregivers and providers, which happened whenever we were able to get them,” said Tonya.
As COVID-19 cases rose steadily in St. Louis throughout early December 2020, SSM Health St. Louis University and SSM Health Cardinal Glennon partnered together to ensure appropriate access to care. Small numbers of COVID-negative, strategically appropriate adult patients were transferred from SLU to SSM Health Cardinal Glennon to allow more open beds for COVID positive adults at SLU. One of those patients was Colton. Colton was transferred from SLU to Cardinal Glennon’s Pediatric Intensive Care Unit on December 10, 2020. His comprehensive team of specialists looked backwards and forwards with regards to Colton’s plan of care. “I was finally able to see my son,” said Tonya. “Cardinal Glennon allowed one visitor in the PICU, so we were elated as a family that we could finally talk about Colton and his care face to face with his team,” Tonya said. “Everyone at Glennon was amazing at explaining his care in detail. We were constantly asked if we had any questions, and we spoke at least once, if not multiple times per day with his doctors,” Tonya said. “Colton had pneumonia, persistent fevers even though his E-Coli infection cleared, and he was still not responsive to commands. We were worried that he might have been falling through the cracks before he transferred to Cardinal Glennon. It was reassuring to be able to see such attentive eyes on our son,” said Tonya.
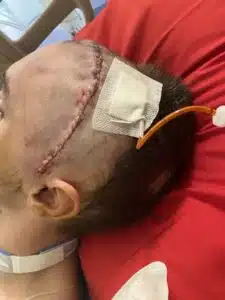
Dr. Philip Mercier, the neurosurgeon involved with Colton’s case reviewed and inspected one of Colton’s former brain scans. Looking at the scan, he suspected that Colton had an abcess in his brain that could potentially be the source of his persistent fevers and other symptoms. “On December 18th, Colton had brain surgery,” Tonya said. “He had that area of his brain cleaned out that Dr. Mercier found, and a drain placed to catch any remaining infection. We were hopeful that could mean something positive for Colton, and we were anxiously anticipating how he would do after surgery,” said Tonya.
Just before Christmas and approximately 1 week following his surgery, Colton began showing improvement. He started opening his eyes, and squeezing with his right hand on command. The drain that had been placed in his brain was removed on Christmas Eve. Steadily and definitively, Colton “woke up”. There was new hope and faith that his progress could continue. Colton’s progress was SO strong, that his team began planning for the next chapter of Colton’s journey post-accident: rehabilitation. The family was offered opportunity to explore the possibility of extensive rehabilitation at Ranken Jorden Pediatric Bridge Hospital in Maryland Heights, MO, and on January 12, after an emotionally charged and significant few weeks at Glennon, Colton and his family were ready to take that next step. He was discharged from Cardinal Glennon’s PICU and admitted to Ranken Jordan.
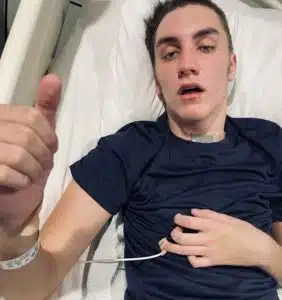
Colton’s quick improvements at Ranken Jordan were nothing short of amazing. After just two days there, he began giving “thumbs up and thumbs down”, signing yes and no to commands, and mouthing words with faint whispers which progressed quickly to speaking. By January 14, he began sitting up on his own, and his tracheostomy was able to be removed.
From January to April 1, Colton was hospitalized at Ranken Jorden Pediatric Bridge Hospital. His days were exhausting yet encouraging at the same time. His day and regimen was full most every day, starting at 7:00am with a shower; 8:00am breakfast; 9:00am-10:00am Occupational Therapy (or Speech); 10:00am-11:00am Speech (or OT); 12:00noon lunch; 1:00pm-2:00pm rest; 2:00pm-3:00pm Physical Therapy; 3:00pm-4:00pm standing and stretching; 4:00pm-5:00pm time with the CPM (continuous passive motion) machine – a machine that slowly and gently flexes and extends the joints after surgery; 5:00pm-6:00pm dinner; 6:00pm-7:00pm group time; 7:00pm bedtime. Colton remarked that the best parts were “water therapy and eating” and the hardest part were “physical therapy”.
When asked what motivates him to get through all of his therapy, Colton joked, “FOOD!” Acknowledging that he loves and looks forward to burgers, pizza and frequent take-out options, he was laser-focused on walking. “I want to walk out of here,” Colton said. “And I want to drive my Charger,” said Colton.
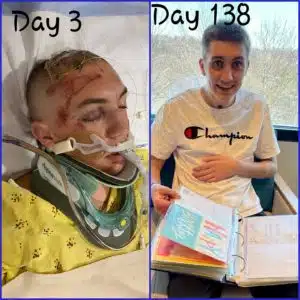
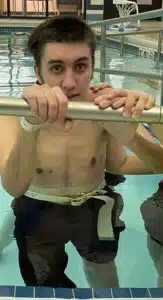
Colton DID walk out of Ranken Jorden on April 1, 2021 from his room all the way to the van. His mom Tonya remarked, “168 days ago, it was hard to see this as a possibility of ever happening. We are just so grateful for how far he’s come. I can’t imagine where we would be today if Colton hadn’t been transferred to Cardinal Glennon. The attention to detail, the compassion, and the faith in what was possible for him has given him his life back. Cardinal Glennon and Ranken Jordan weren’t there to save his life at the beginning; but they never give up on Colton, just like we don’t,” said Tonya.
Since Colton returned home in April, he has been doing physical therapy, speech therapy & occupational therapy 3-4 times a week. He is still unable to move his fingers on his left hand. “His tremors are pretty bad which is effecting his walking, this is his biggest challenge to date. He just really wants to be able to walk. His speech is improving daily. Colton really enjoys water therapy, he said his body doesn’t hurt and he feels like he accomplishes more while in the water. Since being home he has enjoyed friends and family coming and seeing him. Nightly in our prayers we thank Cardinal Glennon and everything everyone has done. If it wasn’t for you all he wouldn’t be where he is today,” said Tonya.
“We have a long way to go, but we’re up for it. I’m pretty sure he is determined enough that he can master just about anything he puts his mind to. We pray for his brain, pray for his memory, pray for
strength, pray for complete healing. We have an amazing community of support,” says Tonya (#coltons_crew),” “and are hopeful for what is to come!”