Our Patients:
Graham Engel

June 2021 – Tori and Zach’s son, Graham (then two years old), started complaining of his belly hurting. The following month, in July, Graham rapidly fell ill after returning home from a family hiking trip to West Virginia. Tori and Zach took him to a nearby urgent care where doctors ordered an x-ray. The x-ray revealed that Graham’s heart was bigger than expected. After a flurry of blood tests at their local hospital, HSHS St. Elizabeth’s Hospital in Shiloh, IL, Graham was transferred to SSM Health Cardinal Glennon Children’s Hospital. Tori and Zach were told he was in heart failure in the early morning hours. Graham was hospitalized immediately, diagnosed with severe dilated cardiomyopathy and remained in-patient for 6 weeks while he received IV (intravenous) medicines to improve the function of his heart. “The doctors thought his cardiomyopathy may have been caused by a virus, but they may never truly know,” recalled Tori.
“We were eventually discharged on oral medications and Graham was thriving at home,” stated Tori. “He started school at Ms. Rubye’s Play Place and was living his best toddler life. Common viruses knocked him down, causing us to return to the hospital a couple of times to get him rehydrated. But all in all, his heart function looked good,” Tori said.
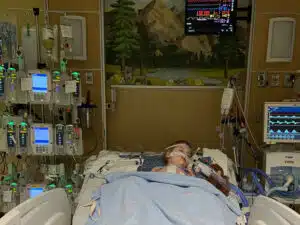
In June 2022, the family took a much-anticipated trip to Disney World, where Graham got to FINALLY meet Mickey. “It was magical,” recalled Tori. “Unfortunately, though, he fell ill several days into our trip. After being transferred between Orlando hospitals, we discovered that Graham’s heart function was dangerously low. They flew us back to St. Louis as soon as possible, where Graham’s condition worsened. He hadn’t seemed that sick in Orlando, but now he was really struggling to breathe. It was terrifying to watch. He couldn’t get comfortable, and it took him so much effort just to breathe – he was using all of his reserves,” Tori said. Graham was quickly placed on a ventilator, then ECMO (extracorporeal membrane oxygenation) – a way to oxygenate his blood and circulate it for him. His heart was exhausted – struggling to keep up with the demands on his body. He was officially put on the heart transplant list on June 16, and on June 18, Graham had a 12-hour open heart surgery to place a BiVAD (biventricular assist device). There are two basic types of VADs: a left ventricular assist device (LVAD) and a right ventricular assist device (RVAD). If both types are used at the same time, they are called a BIVAD. The BiVAD is a pump that helps both the right and left ventricles move blood through the heart.
Graham would remain in the hospital until a heart transplant was available. “We were told we could be waiting anywhere from 6-12 months,” Tori said. The weeks following Graham’s BiVAD placement surgery were a roller coaster and brutal. They were filled with chest tubes, central lines, nasogastric tubes, withdrawal symptoms from pain medications, fluid imbalances, and so many other challenging things too numerous to list. Despite these hurdles, the blessings were great. Graham was able to transition to the Berlin heart (a type of BIVAD with shorter external tubing and pulsatile flow, allowing greater mobility and temperature regulation) on July 5th. The entire staff- nurses to occupational therapists, physical therapists, Child Life therapists, and more – remained creative, innovative, and vigilant in their efforts to keep Graham safe, mobile, and entertained. Surgical recovery transitioned to navigating weeks and months of “life” in the Pediatric Intensive Care Unit.
“Learning to parent a 3-year-old boy in a hospital with two large devices coming out of his body that is run by a large computer (airplane trolley cart size) that requires constant electricity is tricky,” said Tori. “He had candy, snacks, hotdogs, whatever he wanted and whenever he wanted so we can keep his calorie intake high and encourage him to eat by mouth! His days were filled with all things Cars – hiding cars around the unit, racing them on any surface he could find, doing Cars-themed crafts, and reading Cars-themed books. Graham was able to experience some much-needed distractions with the help of his army of caretakers. He loved going to the playroom, and his team coordinated getting him outside when the weather permitted. “Little did Graham know how much of a production it was to get him out of his room,” Tori recalled. “The machine that ran his BiVADs could only be unplugged for 30 minutes. At first, it took him about 20 minutes to walk halfway to the playroom. We eventually got it down to under 8 minutes. We would always take a wheelchair in case we cut it close on time and needed to speed up the process. It takes 6 hours for the machine to recharge fully, and the locations with outlets were limited. We all breathed a sigh of relief once we got to his location and his device plugged into a working outlet. I cannot say it enough – the PICU, Cardiology, Cardiothoracic, Therapy Services, and Child Life staff consistently went above and beyond to normalize his life and get him out of his four walls,” said Tori. “Graham was continuously surrounded by so much love. The nurses were true MVPs, always coming to play and interacting with Graham. The music therapist and child-life specialist worked with Graham to help him express his big feelings. And THOR – Graham grew very fond of the service dog, Thor. He lit up every time Thor and his handler, Abbie came by! I appreciated every moment I got to spend with Graham. He was awake, alert, happy, ornery, joking, and FULL toddler! We know that not every parent can “enjoy” those kinds of moments during their wait. We are so very grateful we had those. At the same time, we were trying to process anticipatory grief for the family, who would ultimately gift Graham with a new heart,” Tori said.
September marked three months. “In the grand scheme, we were told we could expect a 6-12 month wait. I saw parents in online groups who were approaching a year’s wait. Nonetheless, it wasn’t easy,” said Tori. We received a book called Ben’s Zipper: The Story of Ben’s New Heart. It tells the story of a baby elephant that needed a new heart. Graham requested to read it several times It paralleled Graham’s heart journey, and it was a conversation starter about what was happening to him. The book explained that Ben’s new heart would come from Angels. I thought it was a beautiful way to explain it – simple but true. Graham started to echo that when we talked to him about his new heart,” said Tori.
For the most part, Graham continued to have good days. Many days, Graham’s doctors didn’t have much to say. Tori, Zach, and Graham simply “lived” in their room. There were occasional concerns with fever and infection, both of which pose multiple risks. Among other things, they can impact the BiVAD and the effectiveness of medicines, which in turn can increase the risk of stroke. If infections were suspected, Graham got the infection test “buffet: which included nose swabs, BiVAD site swabs, blood cultures, and urine cultures.
“The call came on Thanksgiving day, said Tori. “We were over the moon that Graham would receive a heart transplant, but simultaneously, our hearts were breaking for the donor’s family. We would be forever grateful for Graham’s second chance at life, and for the selfless act of his donor’s family. We received the call while cutting the pie at our thanksgiving dinner in the PICU conference room. The tears continued to flow for several hours. It was shift change at the time of the call. Hug – tears – hug – tears. I laugh a little because I’ve become a hugger in the past year. A couple of days later, on November 26, Graham had a successful transplant. He was extubated quickly and was soon tube free!”
The last phase of Graham’s hospital stay included monitoring his vital signs, blood levels, and nutrition. Graham began eating and drinking well. The team quickly figured out the correct dosage for his transplant medications. On Dec. 5, Graham transferred from the PICU to the Transitional Care Unit (TCU). He had his first post-transplant cardiac catheterization and biopsy on December 7 and was discharged home on December 9. “When I was trying to coax Graham into the car for his first clinic visit after discharge, he commented, ‘I want to stay home forever,’” laughed Tori, “I couldn’t blame him.”
By the end of December, – Graham’s appetite and energy were on the rebound. He was running and playing constantly and started climbing, which was a new milestone. He continued to expand his pallet (though cheese toast and bacon were still at the top of his favorites). The family of three had an intimate Christmas holiday at home.
In early January 2023, Graham had his second post-transplant cardiac catheterization and biopsy. He also had a stent placed due to the pressures around where his new heart was attached. “This was our first overnight stay back in the hospital since transplant. Graham asked if he could stay in his first hospital bed (2504 in PICU) because he said it was fun,” Tori remarked. “It spoke volumes that he thinks so highly of that time.”
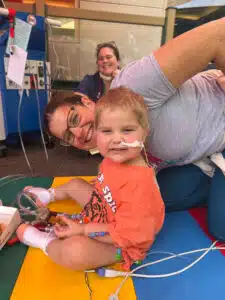
Graham has had no rejection noted from his two biopsies. His new heart is working beautifully. During a warm winter day recently, he went to the zoo and played outside with no wires for the first time since June 2022.
At the end of January, Graham contracted his first virus since transplant. “We are definitely navigating a new world as we figure out what an illness looks like on him,” Tori said. “We were admitted to TCU. Thankfully he didn’t have major respiratory symptoms. He did have a lot of GI issues, though, which kept him under observation in TCU for several days. The only plus of going to the hospital is knowing we are always surrounded by the most caring, talented, and thoughtful individuals. They weren’t just Graham’s care team. They became a major part of MY support system. They understand this language and culture I had been forced to learn and navigate. We shared so much together. Friends and family can’t grasp all that happened within those walls during those six months. It was incredibly difficult to leave that when we were discharged after transplant. Pediatric healthcare workers always put the kids first, but the amount of effort they put into making sure families are part of the decision-making team, informed, and supported is truly under-appreciated,” says Tori.
From Tori and Zach: “We will honor the life of Graham’s donor and the bravery of their family. We are forever grateful for Graham’s second chance at life. We are thankful for those who have prayed, celebrated, and mourned with us. We are grateful for those who sent good vibes for Graham, for dinners, chats, books, toys, and coffee. We are thankful for texts of love, well wishes we haven’t replied to, and much, much more. Graham is running around the house as we write this. There is no way we would be here without the brilliant practitioners who always gave their all to their patients. To the PICU, Cardiothoracic, and Cardiology attendings, nurse practitioners, fellows, residents, pharmacists, nutritionists, nurses, child-life, occupational therapy, physical therapy, food services, and environmental services teams –saying ‘thank you’ will never be enough. You all are forever part of Graham’s story and our story.”