Our Patients:
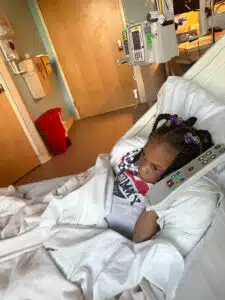
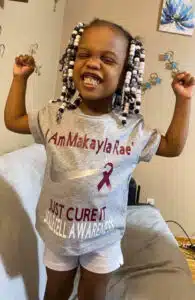
Makayla Cross

When Cheri and Terrion Cross left San Diego in 2016 to come to St. Louis, Missouri, they had been married for two years trying to have children. A blended family, Cheri and Terrion were already parents to teenagers, Elijah and Trinity, but they had hoped for more children to add to their happy home. Cheri found herself blessed with a baby gir later that year, and Makayla entered the world on April 10, 2017. “It was an uncomplicated pregnancy and delivery. We’re from Cahokia, IL and I delivered her at St. Elizabeth’s in Belleville. Terrion and I were thrilled to bring Makayla home and begin enjoying our new normal,” said Cheri.
When Makayla was six weeks old, Cheri received a call from their pediatrician. He informed her that Makayla’s newborn screen came back positive for Sickle Cell Disease. SCD is diagnosed with a simple blood test. In children born in the United States, it most often is found at birth during the routine newborn screening tests at the hospital. Sickle cell disease (SCD) is an inherited red blood cell disorder. Red blood cells contain hemoglobin, a protein that carries oxygen. Healthy red blood cells are round, and they move through small blood vessels to carry oxygen to all parts of the body. In someone who has SCD, the hemoglobin is abnormal, which causes the red blood cells to become hard and sticky and look like a C-shaped farm tool called a “sickle.” The sickle cells die early, which causes a constant shortage of red blood cells. Moreover, when the sickle cells travel through small blood vessels, they get stuck and clog the blood flow. This can cause pain and other serious complications (health problems) such as infection, acute chest syndrome and stroke. Because children with SCD are at an increased risk of infection and other health problems, early diagnosis and treatment are important. People with SCD may start to have signs of the disease during the first year of life, usually around 5 months of age. Symptoms and complications of SCD are different for each person and can range from mild to severe.
There are several types of SCD. The specific type of SCD a person has depends on the genes they inherited from their parents. “We were told Makayla had Type SS,” Cheri said. Neither Terrion or I have the disease, even though we both carry the trait. Our son, Elijah carries the alphathalassemia trait. Our daughter, trinity carries no trait. People who have Hgb SS inherit two genes, one from each parent, that code for hemoglobin “S.” Hemoglobin S is an abnormal form of hemoglobin that causes the red cells to become rigid, and sickle shaped. Hgb SS is commonly called sickle cell anemia and is usually the most severe form of the disease,” Cheri said.
“The world paused for a minute,” Cheri recalled. “SCD is a disease that worsens over time. Treatments are available that can prevent complications and lengthen the lives of those who have this condition. But the treatment options and their effects can be different for each person, depending on the symptoms and severity of their disease. We had no idea how Makayla would do. We just knew this was for life,” Cheri said
“Our pediatrician encouraged us to go to The Costas Center at SSM Health Cardinal Glennon Children’s Hospital and we would meet with a hematologist. Makayla’s first appointment was scheduled for June 2017. That first appointment was informative and overwhelming at the same time. We discussed her treatment protocol and everything we would need to be watching her for at home. We would need to check her spleen, check her hands and feet for swelling, give her penicillin and folic acid every day and try everything we could to keep her hydrated and free of infections,” Cheri said.
In her first year of life, Makayla had lots of illness. In the winter months, she suffered from flu. In the spring, she experienced her first pain crisis. Year two in 2018 was easier, with only one hospitalization in June with fever and pneumonia. “We did everything we could that could maximize her chances of staying healthy,” said Cheri. “We really encouraged her water intake and tried to have her eat more fresh vs. processed foods. We knew processed foods contribute to inflammation, so we tried to bring as many fruits and vegetables to her diet as possible,” Cheri said. “During the pandemic years of 2020-2021, we really tried to stay safe. From handwashing to cleaning to consolidating our trips out, we did our best to keep Makayla well. She also started on Hydroxyurea in 2020 to help prevent pain crises and stroke. Fortunately, she’s never had a stroke, and she has never had an ICU stay.
In 2017, the FDA approved Hydroxyurea to treat children with sickle cell disease. Hydroxyurea makes your red blood cells bigger. It helps them stay rounder and more flexible and less likely to turn into a sickle shape. It increases hemoglobin F, also known as fetal hemoglobin (because newborn babies have it). When you have higher levels of hemoglobin F, your red blood cells are less likely to cause problems.
“In 2022, I started a daycare in my home. It was one of our toughest years for Makayla,” Cheri commented. “Between that, increased traveling and increased gatherings, our year was disastrous as far as hospitalizations. From 2022-2023, she suffered with flu, pneumonia, multiple pain crises and her first episode of acute chest syndrome, Cheri said.
Acute chest syndrome occurs when sickled cells block blood and oxygen from reaching the lungs or may be caused by a viral or bacterial infection. It’s a life-threatening complication in people living with Sickle Cell Disease that can result in lung injury, breathing difficulty, and low oxygen to the rest of the body.
The only therapy approved by the FDA that may be able to cure SCD is a bone marrow or stem cell transplant. “Transplant is an option we will discuss for Makayla. It’s definitely something to explore with her team,” Cheri said. I know we have a great team in our corner with the staff in The Costas Center and on 4 North. They are always responsive and I know I can bring any concern to them any time, knowing they will listen and have the same concern for Makayla’s well-being as me,” said Cheri. “They are always friendly, caring and welcoming during our visits and they respect our lives as busy parents being on-task and offering support. Even though our experience with Makayla has brought her and our family some challenges, our experience with The Costas Center and this disease has inspired us to help others. So many families need basic support. Our family puts together care bags that have things these kids need like water bottles, heating pads, and comfort items for their hospital stays. We’ve also made superhero capes for the patients. These kids are truly warriors,” Cheri said. “We are so grateful for community members who support the hospital and who donate blood. Blood donations and community support literally change the lives of sickle cell patients. Simple things that others take for granted like running or playing outside can turn into a sickle cell crisis in a heartbeat. A blood donation can save a life, and Cardinal Glennon is truly the best children’s hospital, said Cheri. “Makayla wants to be a firefighter when she grows up. With luck, God and continued excellent care, we certainly hope we are able to see her do that!”