Our Patients:
Max Ernest
Jessica and Mykel Ernest from Poplar Bluff, Missouri were happily expecting their second child in early 2019, when the unexpected happened. At 20 weeks and 6 days, Jessica began losing amniotic fluid. This was devastating news to the couple, as both knew the risks of this happening so early in her pregnancy. Though she was dilated to 3cm, Jessica was NOT experiencing any contractions, and her local obstetrician continued to monitor her in the hospital, in hopes that the leak would re-seal. Jessica remained in the hospital on bedrest for the next five days to receive IV antibiotics. There was no further dilation, and the leak slowly decreased over that time.
During that time, however, Jessica and Mykel began their first conversations about what could happen if labor ensued, and they both agreed they wanted all resuscitative efforts done, should their child come early. After five days in the hospital, Jessica was went home on bedrest. Five days after that, Jessica had a “gush of fluid” that puddled on the floor, and she made a frightened call to the labor and delivery unit from which she had just recently been discharged.
She returned to the hospital, where an ultrasound revealed an extremely low amniotic fluid index. That night, at 22 weeks and 2 days pregnant, Jessica was transferred by ambulance to SSM Health St. Mary’s Hospital, where she began receiving steroid shots because the baby’s lungs were still not fully developed. Two days later, Jessica began having contractions and the next day, Friday, she developed a fever, a high white blood cell count and tachycardia. Testing confirmed she had developed chorioamnionitis, a bacterial infection affecting the membranes that surround the baby and the amniotic fluid. On Saturday, it was decided that Jessica needed to deliver, and the staff began to prepare her for what might happen. Jessica recalled, “They prepared me for the possibility that our baby might not survive delivery,” she said.
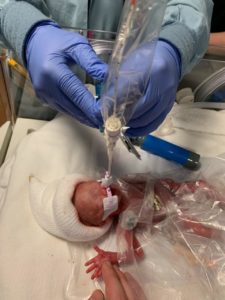
At only 23 weeks gestation, Max was born at 3:07 p.m. on Saturday, February 9. He was 11 inches long and weighed 1lb. 0.1oz. He was whisked to the corner of the labor and delivery room by the staff, where they assessed him and attempted to place a breathing tube. “After the second failed attempt at tube placement, I was told to prepare for his death, as they might not be successful”, Jessica said. “They did get one in, though, and they started getting him ready to send to Cardinal Glennon.”
Jessica had her own issues after Max’s delivery. Her white blood cell count had skyrocketed to 44,000 from the chorioamnionitis and had trouble delivering the placenta. She received a blood transfusion and was immediately taken to surgery as Max was being prepared for transport. The Cardinal Glennon transport team was able to bring Max to Jessica just before they left, giving her a transport towel to wear so that he could have something with her scent until they could be together.
Jessica recalls, “It was all so surreal. It’s hard to remember details, but I remember he was alive and fighting. I knew the NICU at Glennon had NicView cameras, and I couldn’t wait to be able to see him,” she said. “I first logged on to see him at about 1:00 a.m. and Mykel and I watched him for 3 solid hours! I knew my father-in-law was with him, but I hated that I couldn’t be there. Being able to see him through the camera meant everything,” Jessica said. Three days later, Jessica was able to join Max at Cardinal Glennon, and hold him for the first time. Holding him was nothing short of challenging. “He was intubated, with a ventilator, umbilical lines, and intravenous lines for IV nutrition, just to name a few things. His first seven weeks were focused on survival. I remember the neonatologist telling me, “He’s likely going to get a lot sicker, before he gets better,” Jessica said. Shortly after that conversation, that is exactly what unfolded. Max experienced an esophageal perforation when an attempt was made to place an orogastric tube for breastmilk feedings. Those feedings were put on hold and Max was placed on ten days of IV antibiotics. Max had two additional bowel perforations after that. For both of these, the surgeries were performed in the room at his bedside; the first surgery in the middle of the night, and the second during the day. All this happened within the first 16 days of life!
While his bowels rested and healed, Max’s lungs were fighting their own fight. Though he had been receiving hydrocortisone since birth, he had PIE (prematurity-induced-emphysema). His oxygen requirement continued to rise, as did his Co2 levels. Multiple ventilator options were tried to no avail, and stronger steroids were discussed, but avoided due to the potential impact on his fragile bowels. “We all knew steroids couldn’t grow him new lungs. They would just help with the inflammation so that his lungs could be more efficient,” Jessica said. “I remember being scared and asked my neonatologist, ‘Have you ever seen such a small baby with lungs this sick go home?’ His response to me was ‘yes, and I have faith to expect Max could do the same,’” said Jessica. Eventually a stronger steroid was started, and within a week, Max made a complete turnaround, with no untoward effects to his bowels.
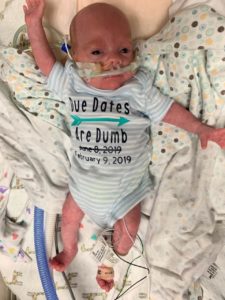
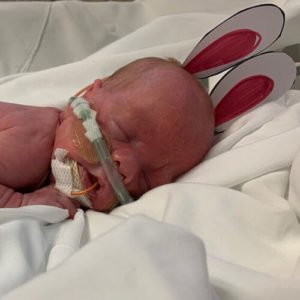
The next several weeks were a rollercoaster of successes and challenges. Jessica never left the hospital; she and Max experienced Valentine’s Day, St. Patrick’s Day, Easter, and months of time together in their hospital room. Living over two hours away in Poplar Bluff, husband Mykel and their older son, Jack, visit each week. After almost three months, Jessica has formed many bonds with the staff – everyone from the nurses and doctors to the housekeepers, maintenance staff, lab technicians, and more. Jessica, a nurse herself, credits the staff with making her journey here tolerable. She says, “The people here invest in their patients and the parents. My faith has definitely grown since I’ve been here, and the little things that people do mean so much. I have so many examples of gestures and amenities that have impressed me. Nurses have created custom onesies for Max, did an Easter photo shoot with him, gave him an Easter basket, and welcomed him to the ‘3 Pound Club’ with a sign on his door. I have taken advantage of the Parent Support Group, the Nic View cameras, and the Ronald McDonald House and Family Room. Staff use every opportunity they can to teach me something, and they are constantly asking me if I need anything or just need to talk.”
There is still a long journey ahead, but currently, Max is making great strides. He is doing infant-driven feedings (both breast and bottle feedings), he is weaning from his CPAP (continuous positive airway pressure), and he has plenty of snuggle time with mom. Jessica is most looking forward to taking Max outside for the first time, and making plans to go home. Just before Mother’s Day, another of Jessica’s highly anticipated wishes came true. Her older son, Jack, was willing and able to hold Max for the first time. Jessica is thankful for the amazing care Max has received at Cardinal Glennon, and just as thankful for the donors that support it. “From the atrium and kid-friendly spaces, to the meal tickets for breast-feeding moms, everything here has been a blessing. We still have a way to go, but I draw strength from Max, and we’ll do it together.”