Our Patients:
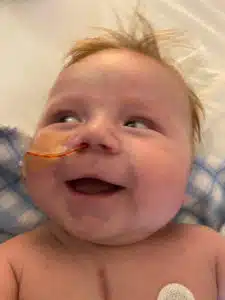
Noah Townsend

Kristi and Eric Townsend from St. Peters, MO were married in 2018. Having married later in life, they knew they wanted to start a family right away. For nearly two years their attempts were unsuccessful, despite rounds of testing and infertility treatments. The couple had almost resolved themselves to believe they would never have children when Kristi turned up with a positive pregnancy test in February 2020.
“My pregnancy was pretty normal at first. I didn’t have much morning sickness, and for the most part felt pretty good. We took a trip to Myrtle Beach in June, and were looking forward to our 20 week ultrasound when we returned. Little did I know how much that ultrasound would change our lives,” said Kristi.
Many couples typically choose to be together for that pivotal 20 week ultrasound. Due to COVID-19 restrictions, Eric made plans to stay in the car, while Kristi went inside the hospital for the appointment. Neither thought it would take especially long, and they both eagerly awaited and expected nothing but a positive report. “I will never forget that day,” Kristi said. “The ultrasound seemed to take forever. I remember the tech telling me it was a boy because Eric and I wanted to know. But I remember her taking an especially long time exploring his heart area. She explained that it was taking a long time by saying, ‘The heart can be tricky’, but I was beginning to feel nervous as the minutes kept passing. I didn’t have my phone to call Eric, and I remember wishing so badly that he was with me. Something didn’t feel right,” Kristi said.
The ultrasound tech left the room for approximately 15 minutes, but what seemed like forever to Kristi. She returned to take several more ultrasound pictures, and then informed Kristi that the MFM (maternal fetal medicine) doctor wished to speak with her. The tech escorted Kristi to a waiting room, and then subsequently to an office where she would speak to the MFM via zoom. “It was all so surreal. I was scared, Eric was out in the car, and I no idea what this doctor was going to be telling me about our baby,” Kristi said. “The doctor greeted me on zoom and began talking about what he saw on the images. He started with the positives saying the baby’s size and head looked good. Nothing could have prepared me for what he said next. He told me that he was concerned about the baby’s heart, and that he suspected a condition called Epstein’s Anomaly. He wanted to refer me to SSM Health Cardinal Glennon…..immediately,” said Kristi.
“At that point, MY heart sunk. I immediately excused myself and broke down in tears. Is my baby going to live? Now what do I do? The uncertainty of it all was overwhelming,” said Kristi. “I almost couldn’t breathe as I tried to navigate my way out to the parking lot and find Eric. I remember just being in a daze the whole way home, having no knowledge of what I was just told, or really what to expect next,” Kristi said.
“Someone from SSM Health Cardinal Glennon called me that day. It was a Friday afternoon,” recalled Kristi. “They told me that Dr. Gloria Lehmann, a cardiologist, had an opening to see me on Monday. While I was grateful that was soon, it seemed like torture to wait. It was the longest 3 days ever until that appointment time arrived.
Kristi and Eric met Dr. Lehmann that Monday at the St. Louis Fetal Care Institute at SSM Health Cardinal Glennon Children’s Hospital. It was just down the hall from the Dallas Heart Center. Both places would become a second home over these next several weeks and months. Kristi had a fetal echocardiogram – the first of several in her future, which confirmed the baby’s diagnosis of Epstein’s Anomaly and Pulmonary Atresia. “Hearing it confirmed was so hard for Eric and me,” said Kristi. “We were still trying to process that something was wrong with our baby.”
Despite the agonizing confirmation of what they already had been told, there were many things during that first visit that were reassuring and comforting to Kristi and Eric. “Dr. Lehmann drew us photos of EVERYTHING to help us understand,” said Kristi. “She gave us statistics, a care plan for the rest of the pregnancy, and she presented us with multiple scenarios and surgery options, which would all be discussed in deeper detail as the weeks of the pregnancy unfolded,” said Kristi. “We also met Dr. Fiore, who would eventually be our baby’s heart surgeon. He was nothing short of amazing, and his confidence was just the reassurance we needed,” said Kristi.
After that first appointment, Kristi visited her obstetrician every week for ultrasounds, stress tests and growth measurements. She and Eric visited the FCI every four weeks. “They monitored the baby’s growth and development, the baby’s blood flow, and my symptoms. I found myself looking forward to appointments because I actually got to SEE my baby and he was growing and doing well,” said Kristi. “Dr. Lehmann made sure she was there for EVERY FCI appointment and ultrasound. She would continue to draw pictures and reinforce information she had already shared. I appreciated that she did that every time, because hearing it over and over really helped us understand our baby’s diagnosis, and what things were being planned for him,” said Kristi.
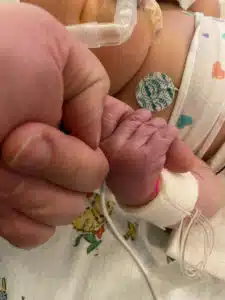
At her 38 week ultrasound, Kristi’s obstetrician noted that her amniotic fluid was low. They immediately planned a labor induction and delivery at SSM Mary’s Hospital in St. Louis. “Everyone at St. Mary’s was amazing. There were a ton of people prepared and ready for me and the NICU was on standby. After a 3 hour labor, Baby Noah was born at 7:03pm on 10/22/20. Kristi got to hold him briefly, and Eric was able to cut the umbilical cord. Their time together didn’t last long; however, Kristi was wheeled back to postpartum and Noah was placed in an incubator to get prepped for transport to SSM Health Cardinal Glennon. “I knew he wasn’t going to come back to me in my room,” recalled Kristi. “I felt like I was in such a daze, but I remember watching the transport team arriving with all of their equipment. They were placing his incubator on their gurney and doing everything they could to keep him alive to get to Cardinal Glennon,” said Kristi. “Eric went home that night to rest for what would be a crazy day the next day. I spent the night at St. Mary’s listening to the innocent crying of other babies, trying to process what had just happened.”
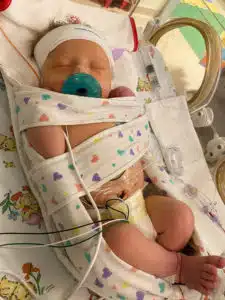
Kristi was released from St. Mary’s the following morning, and she and Eric bravely walked through the doors of Cardinal Glennon’s NICU for the first time. “I know they prepared us for all that we might see, but I don’t think anyone can truly prepare you for seeing your baby hooked up to so much. He had intravenous lines, arterial lines, CPAP, and so many monitors. It was so busy in there and there was a lot of activity – everyone making sure that Noah was getting everything he needed,” said Kristi. During pregnancy, I think I had a little bit of denial. He was doing so well with his development, so I thought maybe this wasn’t real or that his case wouldn’t be severe. That first day in the NICU was eye-opening,” said Kristi. “This isn’t how most moms spend the first day with their baby.”
Over the next few weeks, some of the technology and monitoring as part of Noah’s care became less intense. Many bonds of trust were formed with the nurses and physicians – trust that gave Eric and Kristi confidence to go home at night, knowing Noah was safe and loved. “It’s really hard to leave and go home. But knowing Noah had such a good team gave us the reassurance we needed to take care of ourselves, too. COVID restrictions made it difficult and isolating to go through this whole process. That time to be together in our own home at night was important for US,” Eric said. Eric and Kristi also had regular conversations with Dr. Lehmann and with Dr. Fiore, Noah’s cardiothoracic surgeon. Kristi recalled Dr. Fiore saying, “If he has to live with half of a heart, it’s fine! We can make it work. If he needs a transplant, that’s ok too!” There was a lot of deliberation about the direction to take with his first surgical intervention. Ultimately, it was decided to delay a full repair until Noah was older. He was doing well enough to allow time for him to grow, and a smaller surgery would carry less risk. “Having those regular conversations with Dr. Lehmann and Dr. Fiore were SO valuable. We had met them before Noah was even born, and built trust. As we kept moving through Noah’s first few weeks of life and time in the NICU, just having them check in on us was so reassuring,” said Kristi.
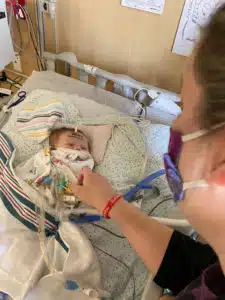
Noah’s first surgery – a shunt placement – was on 11/4/20 “Dr. Fiore prayed with us the morning of surgery. I remember the words he said,” recalled Kristi. “He said: Let Noah be safe. Let me have steady hands.” ”His faith and confidence meant the world to us,” said Kristi. Noah’s surgery lasted several hours. Nurses prepared Eric and Kristi as best they could for what expect in the PICU (Pediatric Intensive Care Unit) that afternoon and in the days to follow, but both Eric and Kristi commented that “no one tell you how much it guts you.” “When they told us surgery went really well, we expected to just see him sleeping,” Kristi said. “It was devastating to see him so swollen, so dependent, the breathing tube and machines helping him breathe, and so many IV’s and pumps,” said Kristi. “We knew, though, that he was in the best hands possible, and that he was safe. At any given point there would be 15 people in the room if one of his nurses called or help,” Kristi said.
Noah’s recovery went well in the PICU. Eventually he transferred to the TCU (Transitional Care Unit) where the goal was to prepare for going home. “So much happened on the TCU. It was there that I had to start learning how to be a mom. Being Noah’s mom meant learning a lot extra on top of what other moms learn, like being trained in CPR, trained in changing bandages, trained in feeding techniques and inserting feeding tubes, trained on how to monitor his oxygen saturations and trained on equipment. It was a lot. We met nearly all of the cardiologists during our stay there, but it was always a huge blessing when Dr. Lehmann would come by to check on us. She would make regular visits even when it wasn’t her rotation. She always made sure she answered all of our questions, and she never made Eric and I feel rushed. We felt like we were her only family to take care of, and that we mattered. She was invested in us, and in Noah,” said Kristi. “I don’t tend to cry, but I could cry with her. I also remember leaning on Noah’s nurses like Brooke and Diane and Nykesha. They were all so understanding, and so patient as I learned Noah’s care. I had to rely on them a lot,” said Kristi.
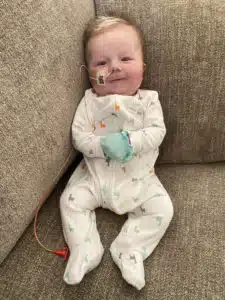
Noah was eventually discharged home on 11/17/20. “It’s been quite the balancing act since then,” Kristi said. “Eric and I both work full time (from home due to Covid). Juggling work while managing Noah’s care isn’t always easy,” admits Kristi. “Noah has monthly cardiology appointments in the Dallas Heart Center. We have some feeding struggles with him, and we are always on the alert watching for signs that his heart might be working too hard. It’s a roller coaster of emotions, and we’ve learned not to be shy about following our gut or asking too many questions, said Kristi. “One of the hardest things is realizing how hard it is to plan anything. I’m a planner, and I’m realizing that Noah is the one in control, not me,” said Kristi.
Noah was in and out of Cardinal Glennon for feeding difficulties in late January and early February 2021. Eric reported when Noah was admitted in February it was due to increase lethargy and feeding difficulties. The right side of his heart looked enlarged on an echocardiogram, and he was experiencing right-sided heart failure. He was admitted for monitoring and further evaluation, and it was decided within days to perform a cardiac cath and open his arterial septum a small amount with a balloon. “We’re hoping to put off his full repair as long as possible,” Kristi said. “The hope with this procedure is that we can still buy more time before that becomes our only option.”
In late February, just weeks following his balloon procedure, Noah’s oxygen saturations were falling into the 70’s. He began having a bluish color to him, and was sleeping 20 hours out of the day. His cardiology and cardiothoracic surgery team felt that it was time to perform his Glenn Procedure. A surgery date was set for March 4th.
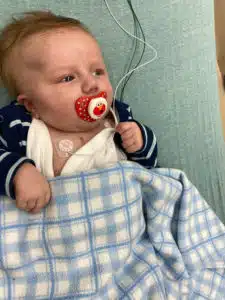
Once in surgery, Dr. Fiore and Dr. Huddleston made the decision NOT to perform the Glenn Procedure, as originally intended; in other words letting him have a 2 ventricle fully functioning heart. Eric and Kristi were extremely thrilled and cried tears of happiness. “It was the most stressful and joyous day of our lives,” Kristi said. When Kristi and Eric were first able to see Noah after surgery in the PICU, he had oxygen saturations between 95-100%, which they had never seen before. Throughout the next several days, they were able to witness a Noah who was pink, and awake and alert more than ever. Noah was extubated on the 3rd day after surgery, and was discharged home on March 12. Eventually Noah will need his pulmonary valve replaced since it won’t grow with him. The hope is that when that happens it will be his last surgery. “It’s really unknown since it’s all based on how Noah does,” said Kristi.
One of the biggest hurdles being home is working on feeding. After several weeks of NG feeding in an attempt to gain weight for surgery, Noah is having to relearn how to take food from a bottle. “It’s working, “Kristi said. “It’s just going to take a bit of time.”
Noah is currently 3 months old, yet Eric and Kristi feel like their bond with Cardinal Glennon extends far beyond that timeline. “If we had to name a silver lining in all of this, it would be that we found out before Noah was born,” admits Kristi. “Even though this journey makes you feel traumatized over and over, there are key people that have been with us from the very beginning. Having the Fetal Care Institute and the Dallas Heart Center available to us, we had the time to process our situation before delivery, and they have grown to know all of us as a family, and be PART of our family. These people just love kiddos, and they HAVE to love what they do because they see babies and parents suffer. We have a long road ahead of us, but we can’t imagine a more supportive team.”