Our Patients:
Ollie Geen

In October of 2021, Jennifer and Brian took their 2 year-old son, Ollie to Urgent Care for a persistent belly ache. He had been saying his belly hurt on and off for a few weeks, but it had gotten worse for him after a fall on the playground. Knowing that COVID could present as gastrointestinal symptoms in toddlers, they wanted to look into his general belly ache for that if nothing else. Ollie had what they characterized as a bloated belly; however it had looked like a “toddler belly” on and off for months. Nothing seemed abnormal.
It was a Sunday morning when Jennifer wanted to take Ollie in, but few if any places were open for appointments. Jennifer and Brian found an opening at an SSM Health Cardinal Glennon Urgent Care. Ollie had vital signs taken, a pulse oximetry test – all of which came back normal. The nurse practitioner felt his belly, sensed something wasn’t quite right, and got an X-ray of his belly. He also got a COVID test, and some Miralax and an enema – just in case it was a case of constipation. Ollie’s COVID test was negative, and the enema produced no results. Twenty-four hours later, on October 25, the urgent care called Jennifer and Brian, telling them that the radiologist wanted Ollie to be seen in the Emergency Department at SSM Health Cardinal Glennon.
A CT scan and subsequent blood work revealed a large mass that was cancerous. “It was the biggest nightmare,” recalled Jennifer. “Complete devastation. Disbelief.” Ollie was admitted that evening to the inpatient oncology unit. He received a blood transfusion that evening as his red blood count was low and an MRI was ordered for the following day to get further imaging of his mass and spine and pelvis area.
The MRI and some additional testing confirmed where the tumor was coming from and the type of cancer it was. The cancer was coming from his liver and called Hepatoblastoma. Surgeons then spoke with Ollie’s parents to discuss tumor biopsy or possible resection the next day..
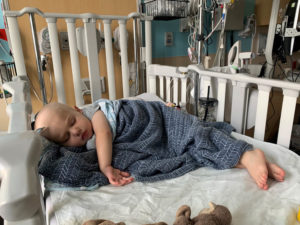
Surgery revealed that the tumor was too close to the portal vein and too vascular to be removed at that time. After more than three hours in surgery, the biopsy was complete and Ollie had a central port placed for blood access and treatment. He went immediately to the pediatric intensive care unit that evening to be closely monitored. “Brian and I were so thankful that we could stay in his ICU room with him. The surgeon said that despite the tumor not being able to be removed, it had not wrapped itself around the portal vein. He also thought that with treatment, hopefully the tumor would shrink and we could get it out (eventually). It was one of the most difficult nights of our life to hear this information and see our baby like that,” Jennifer said.
Within the next couple days, Jennifer and Brian were presented with Ollie’s treatment options. The surgeon and oncologist hoped to allow a few more days of recovery from surgery, but start his chemotherapy the following week. “We had so much information coming at us quickly. He had so many tests, procedures, major surgery. But at the same time, we felt so fortunate to be working with world class doctors who seemed to think Ollie would be cured. We knew we had a long road of treatment and surgery ahead of us,” said Jennifer.
Ollie’s first round of chemotherapy began November 2, 2021 – just 7 days after diagnosis. The goal was to have two rounds, and then scans to check and see if his tumor had shrunk enough to have surgery.
“Some of the known side effects of his chemotherapy were hearing loss and heart issues. We prayed that the chemicals worked to reduce the tumor, but also that Ollie was spared some of these big side effects of the same drugs that were required to save his life,” Jennifer said. “ “Initially, his side effects were pretty minimal. We were happy that Ollie wanted to get up and go for a walk. He also requested ‘his instruments’. He loves playing instruments and the music therapist came by to show him a variety of instruments he could play! A child life specialist arranged for us to get some solo play for him in a special playroom for toddlers, also. He was so happy and kept telling her ‘thank you’. I cannot say enough about how amazing the staff are. Little wins each day definitely helped us stay positive and strong for our boy,” Jennifer said.
Ollie was able to be discharged on November 4. “Home. Sweet. Home. Those words took on a whole new meaning after those first ten days. Life is so fragile and precious. We all know this figuratively but to experience it literally puts things into such perspective. To think of all the things that had to go right for us to be home was really amazing,” Jennifer recalled. “Before we left, the family across the hall from us whose son was diagnosed a week before Ollie – gave me a bracelet that says Faith Over Fear. I couldn’t have said it better myself.”
The next few days, Jennifer and Brian felt themselves re-establishing their “normal”. “Getting a hold on all the medicines was overwhelming,” Jennifer said. “We had to learn what works and what he needed.” Ollie did well with his first outpatient chemotherapy infusion in The Costas Center. “He is such a strong boy when they access the port and draw blood and hook up his IVs. When he was done with his treatment he was surprised to find out he got to pick a toy from the toy closet. This is all thanks to the Friends of Kids With Cancer Organization. I love the nice little touches all around to help these kids cope,” commented Jennifer. “His blood count labs were lower this week. This is to be somewhat expected as we go along – especially his white blood cell, hemoglobin and overall CBC counts. Low counts can impact if we are able to start subsequent rounds of chemo where he will be admitted again. If we are not able to, treatment is delayed. We have to be extra careful since his immune system is very compromised. We also have to watch for signs that he may need a transfusion,” said Jennifer.
“The only way out is through.” As they prepared their hospital bags for a planned 3rd round of chemo and admission, Brian and Jennifer definitely felt anxious. Sometimes the middle is often the hardest. “We had 6 more weeks/ two more rounds (rounds 3 and 4) of chemotherapy before a surgery occurred followed by an additional 6 weeks (Rounds 5 & 6) of chemo after surgery. It was also weighing heavy on us as that it was still unknown if the tumor could come out successfully,” said Jennifer.
Brian and Jennifer met with two very skilled and knowledgeable pediatric surgeons. They were also introduced to the transplant team in case there was a need for them. Over the next several weeks, Ollie’s team prepared everything to list him on the donor list should that be needed. Olliie’s tumor response to round 3 of treatment would be critical to determining his path forward through his cancer diagnosis.
Thankfully, there was significant tumor shrinkage. After round, the tumor was roughly half the size it was at diagnosis. The surgery team felt it could be successfully resected. Ollie would have one more round of chemotherapy late January with a triple phase MRI and CT after that for final surgery prep. The possibility of transplant was no longer needed.
“We are so thankful for the technology at Cardinal Glennon. The triple phase MRI looks specifically at the veins and arteries and how they interact with his tumor. I remember walking out of the imaging area the morning of that MRI. Each morning at Cardinal Glennon over the PA system, they read a bible verse ad say a prayer. That morning, I immediately recognized the verse – Jeremiah 29:11….’For I know the plans I have for you, declares the Lord – plans to prosper you and not to harm you – plans to give you hope and a future…’ I thanked God for this message of hope when we were feeling weary,” recalled Jennifer.
Ollie had fluorescence-guided surgical resection of his tumor on February 7, 2022. Pathology reports from specimens taken during the surgery were positive. Once he recovered from surgery, he would have two more rounds of chemo to complete to ensure that all cancer cells have been eliminated.
“When we were staying in the hospital for round 5, we were thrilled to reunite with Nurse Practitioner, Jenny. Jenny was the NP at the urgent care who had the instinct to get Ollie a belly x-ray. She is also an NP in the ER at Cardinal Glennon! She had the x-ray flagged for further review by the radiologist at Glennon because it didn’t look like traditional constipation. We are so incredibly thankful for her role in saving Ollie. Had we had to wait additional days/weeks to find out what was wrong, Ollie’s outcome could have been much different or fatal,” Jennifer said.
March 29, 2022: Day 154. Round 6. Day 15. Treatment #18. “It was truly hard to adequately articulate the intense feelings of gratitude in a situation that still felt somehow unreal. How do you express to the people and institutions a ‘thank you’ for literally saving your child and giving you hope? March 29 was that day – after Ollie had his last chemotherapy treatment. Tears streamed down my face as we saw our tribe cheering, with bubbles, noise makers, posters. Just WOW. These were the people who had been there through it all – the good days, the bad days, the shock, the tears, the hair loss and everything in between,” said Jennifer. Ollie rang the bell, celebrating completion of the chemo protocol for intermediate risk Hepatoblastoma.
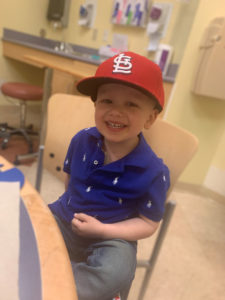
The following week, Ollie had scans which confirmed he was in remission! He would have monthly AFP (alpha fetoprotein) levels (a tumor marker test) and quarterly scans for the next year. He would also be monitored for long term side effects from the various chemotherapy agents he received. In May 2022, the family enjoyed a much needed family vacation in Florida and in June, after 7 months away, Ollie celebrated a return to preschool.
Jennifer comments, “Brian and I are absolutely grateful that we ended up at Cardinal Glennon that day months ago, and thankful beyond measure that they were able to give Ollie the very best chance at a full recovery.”