Our Patients:
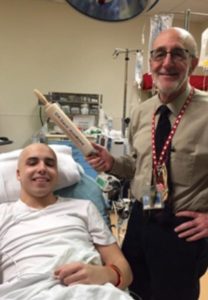
Super Thomas and Uncle Joey

It was, unusually, a gloomy day on 4 North, where doctors and nurses faithfully maintain a cheerful atmosphere for patients undergoing inpatient treatments for cancer and blood diseases. “A nurse said he could feel that something wasn’t right,” says Carol Anne Lorenz. “Then someone told him, ‘Thomas Lorenz is up here — Joey’s nephew.’”
Carol Anne’s 3-year-old son, Thomas, had been diagnosed with acute lymphoblastic leukemia (ALL) and admitted to the floor for the intense, 30-day, induction stage of treatment. Thomas was across the hall from his 23-year-old uncle and Carol Anne’s brother, Joey Renick, who was undergoing treatment for his third bout of ALL in 20 years.
Carol Anne was no stranger to 4 North at SSM Health Cardinal Glennon Children’s Hospital. “It was horribly shocking and sad,” she says. “Joey was just coming out of the scary part of his treatment then we found out Thomas also was sick. There are people on 4 North who have known me since I was little and visiting Joey. They were taking it like Thomas was their kid.”
1996
Diana Sollmann, Joey’s mother, remembers the day her family began to learn about leukemia.
“It was 20 years ago on October 18. I brought Joey to the hospital because he had a fever. After three hours Dr. Gale and our pediatrician told me Joey had leukemia and it would be a very long road — three years of treatment.”
Gordon Gale, MD, was Joey’s first oncologist. When Joey relapsed at age 18, Dr. Gale had become a sedation specialist in the division of critical care and prepared Joey for procedures. He provides that care to Thomas. “I have gotten very close to this family,” says Dr. Gale, a Saint Louis University Medical School professor of pediatrics at SSM Health Cardinal Glennon. “I consider them friends as well as patients.”
“From 3 years old until I was 6 I was in the hospital pretty much all time,” recalls Uncle Joey, as he is known to family and the staff. “There are lots of memories — shots, chemotherapy, spinal taps, bone marrow aspirations, total body irradiation and a few surgeries.”
However, he adds, “Glennon makes a bad situation a little more comfortable. I have known a lot of the nurses for 20 years. They love their jobs. They have had birthday parties for me. I know who is going to see me and I trust them.”
Except for routine checkups, Joey enjoyed a normal childhood of school and sports. “I relapsed for the first time just before my 18th birthday,” he says. After another course of chemotherapy, he was in remission and embarked on a nursing career.
Coincidence
During his second semester of nursing school — February 12, 2016 — Joey relapsed again. “Relapsing a second time is an indication that the leukemia will not be cured with chemotherapy alone,” explains Deepika Bhatla, MD, a SLUCare hematologist/oncologist at SSM Health Cardinal Glennon’s Costas Center and associate professor of pediatrics at Saint Louis University School of Medicine. “A bone marrow transplant replaces the diseased marrow and provides a new immune system which helps fight leukemia cells. A transplant with a second relapse of leukemia is fairly standard treatment.”
Dr. Bhatla cared for Joey when he was 18 and now cares for Joey and Thomas. “They started looking for bone marrow donors,” Joey says. “Usually, one in six siblings is likely to be a potential match. All three of my sisters were.”
When youngest sister Noelle was born her umbilical cord stem cells were frozen in the then-new St. Louis Cord Blood Bank at SSM Health Cardinal Glennon. The cells are collected after babies are delivered and can be used to treat more than 70 diseases, including leukemia. Considered an investigational treatment when Noelle was born, cord blood stem cells are now classified by the U.S. Food and Drug Administration as a biologic drug.
Carol Anne’s mother-in-law, Joan Lorenz, M(ASCP), is a microbiology technologist in the blood bank. Noelle’s bone marrow supplemented her cord cells. “The stem cell number with cord blood alone would have been too small for Joey’s age and size,” Dr. Bhatla says.
Noelle, now 17, underwent a donation procedure. “They used needles to syringe marrow out of my pelvic bone,” she says. “I was in the hospital for a day. I feel really honored that I was able to do this for him.”
ALL
“Acute lymphoblastic leukemia is a fast-growing, white-blood-cell cancer that is in the blood stream so it affects your entire body,” recites Joey. ALL causes the bone marrow, where most blood cells are produced, to create abnormal white blood cells (lymphocytes) that displace normal white blood cells, red blood cells and platelets. The cancer can spread to other parts of the body.
An estimated 6,590 patients were diagnosed with ALL last year — 0.4% of all cancers in the United States, according to the National Cancer Institute. Its incidence is 1.7 of every 100,000 people. “Joey and Thomas have a very common childhood cancer,” says Bhatla. “It is a good-prognosis cancer — one that we have had a lot of successes in treating.”
Little is known about ALL’s causes, she says. “Something happens within the cells that causes them to disobey normal signals. They divide when they don’t need to and don’t die when their job is done. Those cells escape normal immune mechanisms and take over the normal blood cell productions in the bone marrow.”
“It is rare for a second family member to develop leukemia,” says Karen Imperiale, RN, an SSM Health Cardinal Glennon nurse for 39 years and a staff member of The Costas Center since 1984. “It doesn’t happen very often. Thank God.”
Joey and Thomas might lead to better understanding of acute lymphocytic leukemia. Could there be a genetic factor? “I think there is definitely something that we have not been able to uncover,” Dr. Bhatla says. “I hope we can find out so we can make things better for Joey and Thomas and for other people who have this leukemia.”
Role model
With his cancer again in remission, Joey looks forward to resuming nursing studies this fall while serving as a role model for nephew and godson “Super Thomas” who is a fan of comic book hero Superman. “Super Thomas was diagnosed with acute lymphocytic leukemia on Oct. 23, 2016, so we are still in the intense part of his treatment,” says mother Carol Anne, Joey’s oldest sister. “He will be in active treatment until 2019.”
Thomas is the middle of three siblings. Johnny is 5 and Cora is 2. Thomas and Uncle Joey “already had a really special bond,” Carol Anne says. “Thomas has watched Joey go through all his treatment. When we told Thomas he had leukemia like Uncle Joey, he didn’t see it as something scary. Having Joey to look up to has been important to Thomas.”
Science and research
The treatment protocol prescribed for 3-year-old Thomas differs greatly than the plan devised for Joey when he was 3. “There are more drugs, but the drugs that form the backbone of the treatment are still the same,” Dr. Bhatla says.
Dr. Gale adds, “We can do more to tailor therapy to the child’s illness. Genetic characteristics that are measured in the laboratory were not available 20 years ago. We hope to avoid over-treating children more aggressively than they need to be treated and not under-treat children who perhaps need more aggressive therapies.”
Testing for minimal residual disease (MRD) was not available five years ago. “After the 30 days of induction treatment you are supposed to be in remission and all the leukemia cells are supposed to be gone. They do a bone marrow test to make sure,” Carol Anne says. “They found that Thomas was still MRD-positive. Had they not done that testing we would have gone with the low-risk protocol. He probably would have relapsed immediately, which is much more dangerous. They switched his protocol and hopefully that will lead to a better outcome.”
Improving success
The success rate in treating ALL has tripled since 1975 and approaches 90% according to the National Cancer Institute. Chemotherapy was a major advance in leukemia treatment, Dr. Bhatla says. “Since then the pace of progress has been smaller, but smaller is probably expected when it is getting you from 80 to 90%.”
“Even though Thomas is a high-risk patient, he has a really good prognosis,” says Carol Anne. “It is sad when someone tells you the success rate is 85 to 90%, but that is still good. The doctors and nurses say we can’t focus on the numbers. We just have to look at our child.”
During 33 years at SSM Health Cardinal Glennon, Imperiale has watched countless cancer patients reach adulthood. “Probably hundreds. Some come back to visit and bring their own kids. We are fine-tuning the protocols to see if we can make the success rate 100%.”
In May, Joey married longtime friend Caylee Miller. The wedding reception was attended by many staff members from The Costas Center and 4 North. “They are like part of our family,” says Diana. “Our nurses are so close. The doctors call to see how we are doing when they have the weekend off to spend with their own families. The woman who cleans the rooms says a prayer for Thomas and Joey every time she comes in. There are a lot of smart, capable, trustworthy people here,” she says. “You can only feel sorry yourself for a minute when you look around and see all the other kids.”
“I have attended a lot of weddings. It is rewarding,” Dr. Gale says, adding that one reward is the best of all. “Joey and Thomas are here!”