Our Patients:
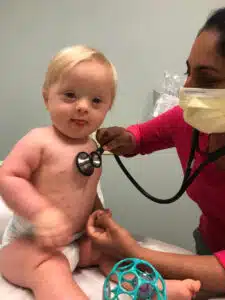
Walker Lydick

When Gretchen learned her unborn son had Down syndrome, she was shocked and scared. Would she love this baby? Would his big brothers accept him? Would he even survive? As a young mom, she wasn’t sure she was equipped to care for him properly, but committed herself to giving him the best life possible — and has since found herself thriving in the role.
The challenges started at the beginning of Gretchen’s third pregnancy, when she experienced frequent, unexplained bleeding. Through visits to her doctor, it was determined her baby had a ventricular septal defect (VSD), a congenital heart defect, and she would need to travel from her home in southern Illinois to be seen at the SSM Health Cardinal Glennon St. Louis Fetal Care Institute.
Gretchen said while she’d declined genetic testing during her previous pregnancies — “It wouldn’t have made a difference to me.” — her doctor recommended it in this case due to the prevalence of heart conditions among babies born with Down syndrome and the close monitoring that would be needed if a genetic condition was detected. Gretchen and her husband agreed.
“Two weeks later we got the news,” she said. It was then that Walker’s parents would first see just how far the team at the SSM Health Cardinal Glennon St. Louis Fetal Care Institute would be willing to go for him and his care. When her doctor called with the results, Gretchen’s husband, a truck driver, was still on the road. She recalls that the doctor stayed on the phone with her for three hours waiting for him to get home so they could all be together. “Never has a doctor been so kind. During that call, he prayed with us, quoted scripture, gave us moments of silence when we needed it,” she says. “He told us this was part of God’s plan.”
Down syndrome, also known as Trisomy 21, is a genetic disorder causing developmental and intellectual delays. It affects approximately 1 in every 700 babies. This extra chromosome affects a baby’s development, resulting in several potential medical issues, including a distinct facial appearance, intellectual disability, developmental delays, and thyroid/heart disease.
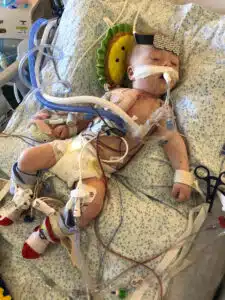
“We were very upset, grieving the baby we were prepared to have,” Gretchen says of their initial reaction. “I feel guilty now about how upset I was, but I think it’s just because I had so many questions. I knew Trisomy 21 was bad, but I wasn’t sure if it was really bad. Would my baby live? The unknown was terrifying.” What followed was a whirlwind of doctors and tests. Complicating things was Walker’s heart condition, which would likely require heart surgery soon after delivery and a six-week stay in the NICU at SSM Health Cardinal Glennon Children’s Hospital. Gretchen was warned that many of the things she’d done with her previous babies — such as breastfeeding and skin-to-skin — would not be possible with Walker. “I wasn’t a first-time mom, but I was a first-time mom for a special needs baby. It was just so scary, but not for one second did I ever think ‘I don’t want this baby,’” she says. “And now that he’s here, he is so perfect beyond anything I ever imagined. The missing piece to my family’s puzzle.”
As her scheduled induction approached, Gretchen prepared her family to survive an extended hospital stay. She packed her bags and sent her two older boys to her sister. Then, the unexpected happened. “I go to have him (at SSM Health St. Mary’s Hospital) and everything is so smooth,” she says. “His heart rate is fine. There were 16 different teams of people in there. I had my husband count, everyone was ready to transport him to the NICU or step in if something went wrong. I was able to do skin-to-skin after all, with the doctors standing very close by. “Walker latched on better than either of our other sons. I was bawling, I was like, ‘You did it baby, they said you wouldn’t!’ and my husband was like, ‘Look, doctors, they’re doing it!’” Gretchen and her husband were able to spend about 10 minutes with their son — “It felt like 2 seconds!” — before he was taken to the NICU. His parents followed close behind.
“I was so scared, I’m prepared to see him with all these cords and devices, thinking I won’t be able to touch him,” she recalls. “But I get there and my baby is perfectly nestled in blankets, no feeding tube, no oxygen, just a standard NICU heart monitor. I was able to breastfeed him there and we got to leave the NICU after just two nights.” From there, however, a new rollercoaster took off.
“He was doing great, eating great, gaining weight … except he wouldn’t pee,” Gretchen says. “Four days old and had only peed three times in his life, when newborns usually pee like crazy.” With concerns about his kidney function and lack of urination, Walker’s doctors wavered on whether they were ready to send him home, ultimately deciding an additional NICU stay was needed. While he was eventually discharged with instructions to follow up with a urologist, around Thanksgiving, Gretchen noticed a mysterious brown mucus in his pee and rushed him back to the ER, where her local pediatrician, Dr. Jones, dropped his holiday plans to come to the hospital and help place a catheter in her tiny one-month-old. “I was told he’d need to be cath’d every three hours,” Gretchen says. “I didn’t think I could do it, I’m not a nurse and he’s a very small baby. But they assured me I could, and I did. I never in my life thought I’d add that to my book of mom skills.”
At two months, Walker was back in the hospital, this time for a vesicostomy to drain his urine, as well as a procedure to release his lip and tongue tie (to help with weight gain). “My other kids are super healthy, so this was a whole new world for us, to just hand him off to the doctors,” Gretchen says. “I got a call soon after the surgery started, the doctor said they’d put a camera down his urethra, which they’d done before, and determined they could avoid the vesicostomy for the time being and just open the urethra a little more,” Gretchen recalls. “This big surgery we were prepared for only took 15 minutes.” The family was discharged within 24 hours and now, Gretchen says, Walker was “peeing like a champ.” “That’s when I knew, my baby, Walker is a warrior,” Gretchen says, adding that Walker did ultimately undergo a successful vesicostomy in March 2022. “He’s going to be a fighter.”
When asked what’s gotten her through a difficult pregnancy and a challenging first few months, Gretchen credits a few key things, including Facebook groups for Down syndrome moms. “I found comfort in them. I have found so many different people in three months, I have literally found a village of people I didn’t even know was out there,” she says, adding that Caleb, her husband and high school sweetheart, has been her biggest supporter of all. Her older sons’ immediate acceptance of Walker was also a great comfort, noting that they helped prepare them with the book “47 Strings.” “We told them that Walker is made with extra love and will be extra special,” she says. “When we asked if they were worried about it, they said no, not at all, if he’s gonna be extra happy. I can’t really explain how adorable it was. They are the best big brothers, they watch out for him.”
Another thing that got her through? A voice she heard in the middle of the night saying Jeremiah 29:11 — “‘For I know the plans I have for you,’ declares the Lord, ‘plans to prosper you and not to harm you, plans to give you hope and a future.’” “I have never received anything like that, that strongly … that right there was from God himself,” she says. “That verse is what carried me through the rest of my pregnancy. I clung to that verse. That is what pulled me through.”
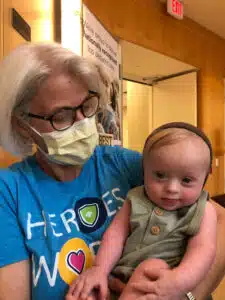
Gretchen says that while she felt at times that her pregnancy was robbed from her, she now believes this is her purpose. “I feel that God has called me,” she says. “God gave me Walker to bring light to other mothers who’ve just received that same terrifying, world-changing news. I want to be helpful, because other people helped me.” Gretchen and her husband are looking forward to giving Walker the best life and showing people in their community just how much is possible for a baby born with Down syndrome. They’ve already started physical therapy and occupational therapy, and will work with the team at Cardinal Glennon to determine what other interventions are necessary as Walker gets older. Walker was scheduled to have his open heart surgery on April 18. He went into heart failure within the week prior; however, so was rushed by ambulance to cardinal Glennon and had his repair on April 15. “It was the scariest thing I have ever been through in my life,” recalls Gretchen. “But on day 5 our little warrior was discharged from the ICU & got to come home. He is healthy, thriving & doing amazing since having his heart fixed,” Gretchen says.
Down syndrome cannot be cured, but early intervention and treatment tailored to each child’s specific situation are helpful in managing this condition. Walker receives all of his care at Cardinal Glennon, which simplifies Gretchen’s life and allows his doctors to develop a comprehensive care plan. Walker has already seen his share of subspecialists thus far including Urology, Cardiology, Cardiothoracic surgery, Ophthalmology, Neurology and Otolaryngology. “The care we get at Cardinal Glennon is exceptional,” Gretchen says. “They’re very supportive and helpful.”
“My advice is take it one day at a time. It’s okay to feel all the emotions,” Gretchen says. “Reach out to other Down syndrome mamas, join groups and do research. There is great resources out there that will bring hope instead of fear & doubt.”
You may see Walker featured in this year’s Glennon Sunday campaign. Click here to learn more about Glennon Sunday!