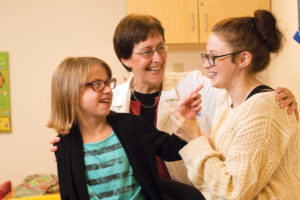Our Patients:
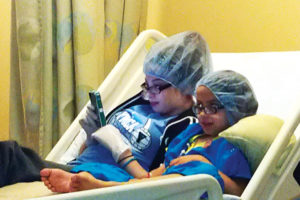
Abbi & Kate Derque

Abbi Derque, 16, and Kate Derque, 10, were born with a rare genetic disorder that is seldom encountered even in a regional pediatric referral hospital such as SSM Health Cardinal Glennon Children’s Hospital. As the disorder’s inevitable and nagging complications progressed, both girls were listed as candidates for kidney and liver transplants – a rarity among the pediatric population. After receiving five years of care at SSM Health Cardinal Glennon, they received the life-saving transplants 11 months apart.
“This is the first set of siblings I have ever done,” says Betsy Tuttle-Newhall, M.D., FACS, surgical director of abdominal organ transplant at SSM Health Cardinal Glennon and professor of surgery at Saint Louis University School of Medicine. “About 20 percent of adult liver transplants also have a kidney, but in children it is not common.”
Tuttle-Newhall says the girls can look forward to productive lives largely due to the support they receive from their family. “They are going to live long lives and have successes and failures like the rest of us,” she says. “They are a little bit battle-worn, but they have got the greatest family. They are very loved and well taken care of.”
“Their mother, Kim Derque, is unbelievable,” adds Ellen Wood, M.D., director of nephrology at SSM Health Cardinal Glennon and professor of pediatrics at Saint Louis University. “She is an incredibly strong person to go through all that she has been through and to be pleasant the whole time. She somehow keeps smiling and going on.”
Kim, on the other hand, credits her ‘new’ family at SSM Health Cardinal Glennon for helping the family endure years of too-frequent hospital stays. “This is almost our second home. We have spent so much time with these doctors and nurses; they are like family to us. I am so grateful we are here. I love this place.”
Abbi was diagnosed with autosomal recessive polycystic kidney disease (ARPKD) when she was 5 months old. The disease was detected in Kate before she was born when an ultrasound identified cysts in her kidneys. ARPKD is associated with liver damage, causing fibrosis or scar formation in the liver, thus preventing proper blood flow. This leads to portal hypertension, a serious condition that can result in life-threatening bleeding. Some children born with the disorder do not survive their first year of life. ARPKD occurs when a child inherits recessive genes from both parents. A child born with only one gene will not develop symptoms. The disease is believed to affect one in 20,000 children. About one in 70 people are believed to be carriers of the recessive gene.
“We searched back on both sides of the family but found nothing that would appear to be this disease,” Kim says. “It might have occurred in previous generations but was just never identified.”
The girls became patients at SSM Health Cardinal Glennon after the family returned to Missouri in 2008.
“ARPKD has both liver dysfunction and kidney dysfunction. The interesting thing is that one of the girls had more liver injury and the other had more kidney injury,” says Ajay Jain, M.D., medical director of the pediatric liver transplant program at SSM Health Cardinal Glennon and assistant professor of pediatrics at Saint Louis University School of Medicine.
“The disease has a wide spectrum,” Wood says. “Sometimes we see people who have very mild disease. They have some cysts in their kidneys but their kidney function is normal. At the other end of the spectrum is the babies who have such severe disease that their lungs don’t develop normally and they don’t have enough lung tissue to support life.”
The disease impairs kidney function by forming microscopic cysts throughout the tubules of the organs, she says. Jain explains that ARPKD injures the liver by interfering with blood flow, leading to hypertension and possibly hemorrhages. “Without transplants their prognosis was very poor.”
Abbi suffered such a hemorrhage on Memorial Day in 2010 and was brought to SSM Health Cardinal Glennon by helicopter. Surgeons placed a stent in her liver and placed her on the transplant list. While the medical team awaited an organ match for Abbi, Kate’s declining kidney function put her on dialysis three times a week beginning in September 2011.
Abbi and Kate developed a second family of doctors, transplant coordinators and dialysis nurses at SSM Health Cardinal Glennon. During the hours she spent each week on the dialysis machine, Kate became a skilled fan of Lego building bricks.
“The sweet Child Life department girls would always stop by during dressing changes and days when she was having a tough time. The iPad and Legos became the best distraction for her,” Kim says. “Last winter when she was hospitalized a resident brought her a huge Lego set that had a hospital, an ambulance and a medical helicopter. You would have thought she had won the lottery! She has a shelf at home with all of her Legos from Cardinal Glennon.”
More family support came into play back at home. Kim’s mother, Hope Cooper, looked out for the children who were not in the hospital when Kim had to be away. “My family has been such a huge help,” she says.
“The need for a matching liver and kidney complicated the search for donor organs,” says Wood. “There would be an offer for one organ but not the other. I don’t know how many times that happened. It took a long time for both of them.”
Double-organ transplants in children and teens also are rare. There were 1,303 organ transplants performed in the U.S. in 2013, according to the Organ Procurement and Transplantation Network. That was 4.5 percent of all transplants.
“In the pediatric population there are 10 to 30 kidney and liver transplants per year worldwide,” Wood says. “There are only a few diseases that require it, and ARPKD is one of the primary diseases.”
Kate was the first to be matched with donor organs. On May 29, 2013, she spent about 10 hours in the operating room. Abbi was transplanted on March 13, 2014.
Liver implantation requires connections with the bile duct and four arteries and veins. The kidney is connected through an artery, vein and ureter.
“These vessels can be quite small in a child the size of Kate,” says Tuttle-Newhall. “Doing a double transplant obviously takes a lot longer than the usual organ transplant. The anesthesia people really have to be on their toes, which they are at Cardinal Glennon, to make sure the patient isn’t overloaded with fluid before we get the liver in.”
“When we do a transplant everyone rises to the occasion. The operating room staff, the nursing staff, the anesthesia people, the blood bank, the instrument room, the pediatric intensive care unit, the hepatologist, the nephrologist – everybody comes together to make it go.”
Kate and Abbi both awoke from surgery with brother Johnathan, now 14, beside them. He insisted that he be present to hold each sister’s hand in the recovery room. The genetic disease skipped Johnathan, but Kate and Abbi had been very sick for about half of his life. “They didn’t feel good a lot of the time. They were always tired and couldn’t do much,” he says. “Things were real tough for them. I wanted to support them until they got better and help them if they needed something.”
“He has been the tough brother,” Kim says. “He was going to make sure his sisters were okay. He has taken all this so well. At one point he said he wished his sisters could have his kidney and liver. I told him he is going to need those.”
More family members pitched in to support Johnathan when his sisters were hospitalized — his uncles made sure he had fans on hand at his little league baseball and football games.
Both girls spent nine days in the hospital following surgery. By the summer of 2014, Kate was more than a year removed from surgery and was a bundle of energy. When asked what the highlights of the year had been, she says simply, “Swimming.” Then she dramatically raises her arms, looks skyward and exclaims, “Chocolate!”
“No more renal diet. No more food restrictions like when she was on dialysis,” says her mother. “Now we can’t keep her down.”
Only a few months away from her surgery, Abbi spent a more peaceful summer, enjoying the freedom to leave the house and visit friends.
After missing a lot of school in recent years, the sisters returned to school in August. Kate is in the fifth grade at Crystal City Elementary and Abbi is a sophomore at Crystal City High School. Their mother returned to school, too, as a teacher.
During the years she led her family through severe illness and transplant surgeries, Kim returned to college. “I graduated from Missouri Baptist University in April,” she says. “I had started working on the degree years ago and just needed to finish it. It kept my mind busy so I wasn’t so focused on everything that was going on. It also, I think, helped us look toward the future.”
Kim’s teaching career began this fall as a teacher’s aide for pre-kindergarten students in the Dunklin R-5 School District. “I am swarmed with kiddos!” she says. “I absolutely love teaching!”
Kim’s girls already are thinking about college, she says. “Abbi wants to be a transplant coordinator because she thinks that is a wonderful job. Kate is talking about being a dialysis nurse because she spent so much time in dialysis.”
Kate and Abbi will continue to take daily medications to prevent their bodies from rejecting the transplanted organs. They will need to visit the hospital regularly for blood tests.
“They have both done really well,” says Tuttle-Newhall. “They have grown a bunch. Any issues they have are going to be related to the medicine they have to take to suppress their immune systems.”
“They can both do pretty much anything they want,” Wood adds. “Because they are immunosuppressed, they will deal with an increased risk of infections and a small increased risk of malignancies.”
“The transplanted livers and kidneys should keep Abbi and Kate going through the rest of their normal lives,” Jain says. “That is the hope and expectation.”
“In the years ahead they will be among the pioneers who will break new ground and discover the longevity of transplanted organs,” he says. “These girls are young – over the next decade or so there will be newer medications and newer interventions that could potentially help them.”
“I’m feeling a lot better. I started getting more energy about a month after the transplant, but I am still healing,” Abbi says. “Next summer is going to be a lot different. We are going to travel more.”
“To have a normal life is wonderful,” Kim says. “While they were going through their difficult days, we were waiting for our big goal of transplants and then after that – life can begin.”