Our Patients:
Amjad Awawdeli
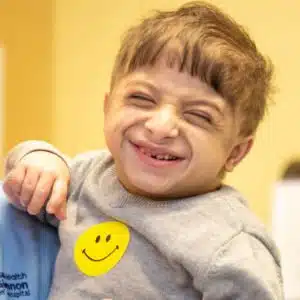
He may be only 26 inches tall, but his size is easily overshadowed by his strength. Six year-old Amjad is almost a celebrity at SSM Health Cardinal Glennon, having won many hearts since he was born.
In 2013, Riki Awawdeli was expecting a baby. Already a mother of three children, she had a history of blood clots during pregnancy and a family history of Familial Mediterranean Fever (FMF). Because of these risk factors, Riki was monitored with a higher than average frequency of ultrasounds and tests.
Familial Mediterranean Fever (FMF) is an inherited disease characterized by inflammation due to an abnormality of the immune system. The main symptoms are fevers, accompanied by painful inflammation in the abdomen, chest or joints. Occasionally, there may also be rash or headaches, or inflammation in other parts of the body, such as the heart; the membrane surrounding the brain and spinal cord; or in males, the testicles. Some children may develop a serious condition known as amyloidosis, in which certain proteins called amyloid accumulate in various tissues of the body. In FMF, amyloid accumulates in the kidneys where it can impair kidney function and potentially result in kidney failure. Not all children have all of these symptoms, and symptoms may change over time. Episodes usually last one to three days, but some children have such frequent episodes they do not fully recover or do not grow properly. Life-long treatment is used to prevent fever episodes and long-term injury to internal organs.
At Riki’s 18 week ultrasound, she was told her baby had high blood pressure and was “smaller than normal” and “not growing normally.” Continued monitoring throughout the next several weeks showed more of the same, but the findings did not outweigh the goal of delaying delivery as much as possible. Finally, at 35 weeks gestation, it was decided to induce labor, and baby Amjad was born via C-section at SSM Health St. Mary’s Hospital, weighing 2lb. 6oz. Amjad was admitted to the NICU at St. Mary’s with a goal of gaining weight and eventually going home. He remained in St. Mary’s NICU for approximately a month, but was never able to tolerate feedings or gain weight. He actually lost weight, and began having random fevers. Amjad’s care team transferred him to SSM Health Cardinal Glennon’s Neonatal Intensive Care Unit. Together, his parents and his care team needed to figure out why he wasn’t able to tolerate feedings and gain weight. Over the next several months, the whole family went through genetic testing, and Amjad had multiple specialists consult on his case. Nothing came from the screen of genetic testing that had been done, other than a positive confirmation of FMF. Since Amjad’s gut had extreme difficulty tolerating enteral or gastric feedings, he had a central venous catheter placed and was fed intravenously with Total Parenteral Nutrition (TPN) and Lipids. Throughout this time, his growth was exponentially slow. He also had complications of line infections and fevers, which added more medications, more tests, and more setbacks to going home. Eventually, Amjad tolerated a minimal amount of gut feeding, and had gained just enough weight to go home. He was discharged from the NICU at five months of age with monthly FMF treatment, nasogastric tube feedings and TPN/Lipid infusions from home nursing at home. Riki recalls the level of support she received for those months from Dr. Farouk Sadiq, Amjad’s primary neonatologist. “He really helped me navigate everything and understand the complexities of all that was going on with Amjad,” said Riki.
On Christmas Eve of 2013, approximately two months after he had been discharged, Riki noticed Amjad wasn’t quite himself. He was more lethargic and sleepy than normal, was breathing faster and sweating. She brought him to the Emergency Room at SSM Health Cardinal Glennon, and he was immediately admitted to the Pediatric Intensive Care Unit. His vital signs and tests revealed that he was in both heart failure and kidney failure, and he was intubated almost immediately after arrival to the PICU. It was suspected his FMF was the cause of his symptoms. Since there is no real treatment for FMF, the care team focused on supportive measures to bring his heart and kidney function back within normal parameters. Amjad remained in the hospital for two months and was able to go home in February of 2014. Amjad acquired a few more specialists that admission, meaning he would now be followed by Gastroenterology, Cardiology, Rheumatology, Genetics, Nephrology and Hematology. He also receives his primary care visits with Dr. Heidi Sallee at The Danis Pediatric Center.
Amjad’s next couple of years were filled with many visits and hospital stays. He suffered frequent infections, central venous line replacements, and consistent feeding and growing issues. SLUCare physician Dr. Stephen Braddock, Director of Medical Genetics at SSM Health Cardinal Glennon, was not convinced that FMF was solely responsible for Amjad’s challenges. Making a diagnosis for a genetic or rare disease can often be challenging, so Dr. Braddock looked back at Amjad’s medical history, symptoms, physical exams, and laboratory test results, eventually deciding to order lab testing for a rare congenital disorder known as Osteodysplastic Primordial Dwarfism. Amjad tested positive for MOPD Type II. This diagnosis helped explain many of Amjad’s physical traits and growth patterns, and was pivotal to understanding what to expect from his health moving forward.
Microcephalic osteodysplastic primordial dwarfism type 2 (MOPD2) is a condition characterized by dwarfism, other skeletal abnormalities, and an unusually small head size (microcephaly). The growth problems in MOPDII are primordial, meaning they begin before birth. After birth, children continue to grow at a very slow rate. Riki states, “Amjad’s height would be a maximum of 52 inches.” Other signs and symptoms of MOPD2 may include hip dysplasia; thinning of the bones in the arms and legs; scoliosis; shortened wrist bones; a high-pitched voice; distinctive facial features (prominent nose, full cheeks, a long midface, and a small jaw); small teeth; abnormal skin pigmentation; and blood vessel abnormalities. Some affected children also have Moyamoya disease, in which arteries at the base of the brain are narrowed, leading to restricted blood flow, and potential for stroke.
Amjad received his diagnosis of MOPD2 at the age of 3. He also has the Moyamoya disease. Both diagnoses reframed his feeding/nutrition goals, and also led his care team to begin preventative screenings for some of the skeletal and blood vessel abnormalities. After suffering a stroke at age 4, Amjad had brain surgery to expand some restricted blood vessels in his brain. Riki is grateful for the consistent presence of Kathy, her Footprints Care Coordinator, who supported her through that difficult decision, and through other difficult conversations and decisions with the medical teams.
In 2016, Riki was encouraged by members of Amjad’s care team to be part of the Complex Medical Care Program. Throughout his young life, Amjad had been seen by many specialists and was also followed by Footprints, our palliative care team. While Riki was initially hesitant to add another team to her son’s list, she quickly realized the value and benefit it would bring to their lives. “Having Dr. Tanios and The Complex Care Team has made it much easier to talk with all of his doctors and coordinate and schedule Amjad’s appointments. All I have to do is call the Complex Care staff, and they handle making sure we can see whoever we need to in the smallest amount of visits possible,” says Riki.
Now in first grade, Amjad is doing well. While most six year-olds have school supplies in their backpacks, the backpack Amjad wears to school holds his nutrition. He is fed continuously for 18 hours a day through a central venous line catheter in his chest with Lipids and TPN, but it certainly doesn’t hold him back. He is keeping up intellectually with his peers, and he receives OT, PT and Speech therapies through his school, as well. He receives a monthly injection for his FMF, and follows up regularly with the GI doctors, and the GIRAF (Glennon Intestinal Rehab and Feeding) feeding team. When asked about next steps for his medical care, Riki says, “It is to introduce food to his gut again, so that he can eventually receive his nutrition there instead of through a central line. He will need to have a feeding tube placed and we will need to start very slowly. There is no date set for that surgery, so until then, the goal is to remain free of fevers and infections,” says Riki. “Fortunately we have been able to graduate from many of our specialists we used to see,” says Riki. “I just want his life to be as normal and as full as possible.”




