Our Patients:
Colten Hong

Watching 9-year-old Colten eagerly polish off a full plate of his favorite breakfast sausages is a moment of joy his mother, Nicole, will never take for granted. For most families, it’s an ordinary morning. For Nicole, it’s a miracle—one she once thought she might never see. Colten entered the world weighing just 1 pound, 11 ounces. Today, he’s an energetic second grader with a big appetite, a full life, and a story that speaks to the power of expert care, unwavering faith, and perseverance through uncertainty.
Nicole’s pregnancy with Colten was filled with challenges from the very beginning. During the early weeks, she experienced significant bleeding and began seeing her obstetrician every few days. Before she reached 20 weeks, a large clot formed in her uterus, damaging the placenta and severely restricting the baby’s growth.
By 20 weeks, it was clear something wasn’t right—Colten was measuring extremely small. Frequent ultrasounds followed, along with genetic testing, which thankfully showed no abnormalities. Still, Colten continued to fall further behind in growth. By 27 weeks, he still measured just under one pound. At that point, a neonatal specialist reinforced the gravity of the situation: if Colten were born at one pound, his chances of survival were about 50 percent. And if he survived, lifelong complications were a real possibility. Determined to give her baby every chance, Nicole began steroid treatments to help his lungs develop and continued close monitoring several times a week.
At 31 weeks, Colten was measuring at just 1 pound, 5 ounces. On October 24, 2016—at 31 weeks and six days—Nicole was admitted to SSM Health St. Mary’s Hospital after a routine appointment revealed low amniotic fluid and suboptimal blood flow. That evening, Colten’s heart rate began to decelerate. Despite medication to slow contractions, an ultrasound the next morning confirmed it was time to deliver.
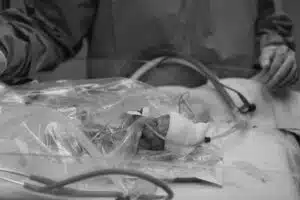
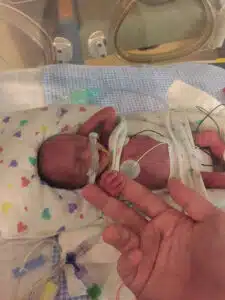
Colten was born via C-section measuring 12.2 inches long and weighing only 1 pound, 11 ounces. Though he had the developmental maturity of a 32-week baby, his size was more typical of a 22-week gestation infant. From the very beginning, Colten showed signs of strength. He was breathing on his own and had a coordinated suck, swallow, and breathe reflex—remarkable milestones for a baby so small. He began his journey in the NICU at SSM Health St. Mary’s before being transferred five days later to the NICU at SSM Health Cardinal Glennon Children’s Hospital for specialized care. Colten had a condition known as intrauterine growth restriction (IUGR) and needed time—lots of it—to grow, learn how to eat, process waste, and avoid infection. There were small but meaningful victories along the way.
“He had his first stool on my birthday,” Nicole recalls. “It was the best present ever.”
Initially, Colten dropped to 1lb. 7oz. after birth, but within the first two weeks, he surpassed his birth weight—a huge milestone—tipping the scale at 1 pound, 13 ounces. He received nutrition through IV and tiny amounts of breast milk through a feeding tube. Every increase was cautious, as his team closely monitored him for complications like bowel perforation.
On November 24, 2016, Colten breastfed for the first time. He had gained a full pound since birth and weighed 2 pounds, 11 ounces. By mid-December, he was taking half of his daily feedings by breast or bottle and nearing the goal of going home.
His NICU stay wasn’t without challenges. Colten experienced a brain bleed that resolved on its own, a small hole in his heart that closed naturally, and hyperinsulinism. Eventually, he was discharged home with monitoring equipment and a schedule full of follow-up visits.
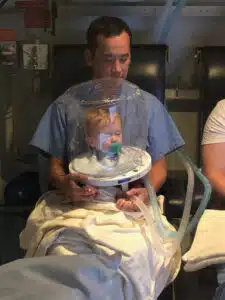
In January 2017, just weeks after coming home, the nanny noticed Colten’s breathing to be rapid and shallow. She and Justen (Colten’s father) took Colten immediately to the pediatrician office, where it was noted that his oxygen levels were dangerously low. He was transported via ambulance to Cardinal Glennon, where he was admitted to the PICU. His underdeveloped lungs needed extra support. After several days of treatment with oxygen, steroids, IV fluids, and a Synagis shot, Colten returned home—this time on oxygen for another month.
Over the next couple years, Colten continued to be followed closely by numerous specialists, including endocrinology, cardiology, gastroenterology, and the NICU follow-up clinic. Therapy was practically a full-time job. For his first two years, Colten received occupational, physical, and speech therapy multiple hours each week.
Eating, however, proved to be one of his greatest obstacles. For the first three years of his life, Colten struggled intensely with feeding. Texture aversion, a sensitive gag reflex, chewing difficulties, and frequent regurgitation made solid foods extremely challenging. Despite normal swallow studies and GI evaluations, Colten vomited after many meals and struggled to gain weight. Determined to avoid a feeding tube, Nicole carefully blended and fortified foods, followed guidance from dietitians, and tried medications to stimulate his appetite. It was exhausting—but she didn’t give up.
Then, during a family vacation in Florida when Colten was three years old, everything changed. “One morning at breakfast, he ate three or four sausage links,” Nicole says. “We were in complete shock.” From that moment on, eating steadily improved. Today, Colten often out-eats his older brother—though even now, at age nine, he remains just below the first percentile on the growth chart. Despite improved nutrition, Colten’s growth remained a concern. After extensive testing, his endocrinology team advocated for Colten to start growth hormone therapy in 2022. Since starting treatment, Colten has been closely monitored every six months. While he has never fully “made the chart,” he continues to make steady progress.
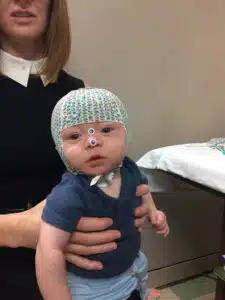
In addition to physical growth, Colten also needed help navigating big emotions. “For such a small guy with such a small beginning, he had big feelings,” Nicole explains. Since 2023, Colten has benefited from behavioral therapy and neurotherapy, helping him build confidence and emotional resilience. Today, he’s thriving in school, forming friendships, and taking part in extracurricular activities—a normal childhood that once felt uncertain. “Seeing him live a life where his time isn’t all therapy and clinic visits anymore is incredibly beautiful,” Nicole says. When Nicole reflects on their journey, her gratitude for Cardinal Glennon runs deep. “The people are amazing. I truly feel the healing presence of God,” she says. “There is such a focus on the family and the caregivers consistently go above and beyond for their patients. Back in 2013, a friend asked me to consider joining the Board of Governors for Cardinal Glennon. I had a tour of the hospital, and as part of that tour, we ironically went through the NICU. I was pregnant at the time with my older son, although no one knew that, and I was able to see a 1lb. baby who had surpassed incredible odds. I marveled at what a miracle he was, and I joined the Board later that year. Fast forward three years later, and we have our experience with Colten. After going through all we did, and continue to, I wondered if God was calling me to be part Glennon’s mission for a bigger reason. After Colten was initially discharged, I asked for a meeting with the leadership of the Foundation and expressed a desire to do something more in honor of Colten, and to be a part of doing something for other families who have to endure a journey such as ours. Our family has since been honored to promote the Homers For Health program each year. This experience has deepened my faith to say the least, and our story is about what’s possible when faith, community, and compassionate care meet an unyielding belief in what a child can overcome.”