Our Patients:
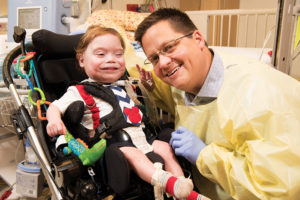
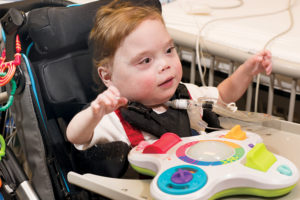
Kevin Lowery

The simple act of playing with a ball might not have been possible without the help of a special device that enables Kevin to breathe easier. Called neurally-adjusted ventilator assist, or NAVA, the system has a unique sensing mechanism that detects electrical activity in the diaphragm whenever a patient wants to take a breath and then helps the patient breathe at exactly the right time.
“It’s a miracle,” says Jennifer Lowery, Kevin’s mother. “It’s lifechanging. It really changed our lives — and Kevin’s — immediately.”
Kevin was born 14 weeks premature when Jennifer had to undergo an emergency cesarean section after she had an abruption, a condition in which the placenta separates from the inner wall of the uterus prior to delivery. That was preceded by a sudden increase in her blood pressure due to preeclampsia.
With underdeveloped and malformed lungs, only one functional kidney and two holes in his heart due to a complex congenital heart condition, Kevin was critically ill from the moment he was born and was immediately transported to SSM Health Cardinal Glennon Children’s Hospital.
“I almost lost Jen and I almost lost our baby,” says Dave with tears in his eyes. Kevin struggled to breathe on his own. He was first placed on a mechanical ventilator, which is programmed to push a breath into a patient’s body at set intervals. But Kevin frequently coughed or gasped at the same time the ventilator tried to push oxygen into his body.
“As you can imagine, when the machine is breathing in a different manner than what they are trying to do for themselves, it’s very distressing and many children are unable to tolerate that,” explains Jason Werner, MD, a board-certified SLUCare pediatric critical care medicine specialist at SSM Health Cardinal Glennon.
“To keep them breathing regularly, we have to keep patients deeply sedated, which blocks the signal from their brain to their muscles. It also means that they can’t really interact with the world around them at all.”
For Kevin’s parents, that meant their baby boy was in a medically induced coma for long periods of time just to allow him to breathe. The cycle went on for months. “If he was awake and trying to exhale while the ventilator was trying to push air in, he would turn blue because he couldn’t catch his breath,” says Jennifer. “But he also couldn’t breathe on his own.”
Just before Kevin turned 1 year old, Dr. Werner brought in a NAVA device on loan from Maquet, the manufacturer. Kevin was the second child to use it.
“Absolutely, there was an immediate benefit,” Dr. Werner says. “With NAVA, Kevin no longer had to be sedated. He was able to be awake and alert, he could move around, smile and interact with his family and play with his toys.”
The game-changer in the design of the NAVA is its ability to sense when Kevin wants to breathe. During normal, spontaneous breathing, the brain sends an electrical impulse to the diaphragm to contract the muscles and pull in air. NAVA continuously monitors for that signal through special sensors and delivers a breath to Kevin at the same time that the signal reaches his diaphragm. The coordination between Kevin’s body and the machine is so precise that NAVA can customize the amount of air needed based upon his own intention.
Jennifer and Dave Lowery say “Super Kev” is doing great after being transitioned to a pediatric bridge rehabilitation hospital and may go home before the end of the year.
“For example, if a baby is asleep and wants to take a nice, deep breath, the ventilator gives him that,” explains Dr. Werner. “Or, if I go, ‘Boo!’ and the baby gasps, the ventilator gives them a nice sharp breath.”
After celebrating his second birthday while in the hospital, Kevin has transitioned to Ranken Jordan Pediatric Bridge Hospital. He has been weaned off of the NAVA device and now is learning to use a traditional ventilator as he continues to recover and gain strength to go home.
Jennifer and Dave now have big plans for their young son. “He’s going to be a musician,” says Dave with a laugh. “My wife and I met in band and we both play instruments. We’re going to teach him to play the piano and guitar.Music’s going to be a big part of his life, I think!” Adds Jennifer, “To have that opportunity to be on the NAVA ventilator changed Kev’s life. He’s here today, able to do what he can do because of that. He gets to be a kid now.”
Dr. Werner agrees. “If anyone wants to know if their donations to the Foundation ever make a difference, they only have to look at Kevin.
Dave looks fondly at his wife and son. “With all of the things Kevin had going on, we didn’t know when, or even if, he was going to come home,” he says softly. “We now have a lot to look forward to. Kev’s got his whole life ahead of him.”