Our Patients:
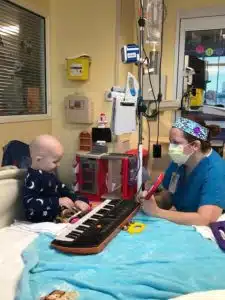
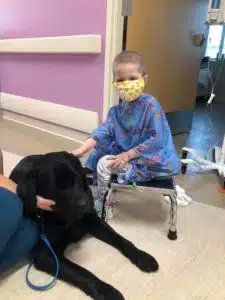
Maren Poettker

Three-year-old Maren, from Aviston, IL was a perfectly healthy, energetic two-year-old, up until October 2019. At that time, she became ill with some persistent low-grade fevers, generally low energy, and a complaint of her neck hurting. At first, parents Neely (Mom) and Chris (Dad) suspected a minor viral process, so they electively kept her home from day care and continued to evaluate her.
After several days passed with no improvement in her symptoms, Neely took Maren to a local urgent care. Maren was pale, and had a swollen, palpable lymph node in her neck. The practitioner encouraged Neely to take Maren to a nearby ED for further evaluation. The physician at the local ED encouraged Neely to have Maren evaluated in the ED at SSM Health Cardinal Glennon. Initial assessment at that Cardinal Glennon visit did not raise concern for anything other than a possible infected lymph node. She was placed on oral antibiotics and sent home.
Maren’s symptoms continued to persist which prompted a visit to their family practitioner. Neely was asked to take Maren to visit the ED at SSM Health Cardinal Glennon for a second time, and on October 17th, Neely’s birthday, Maren was admitted to the hospital for further evaluation and testing. A biopsy of her swollen lymph node was scheduled for and performed the following day on October 18th. Maren’s symptoms improved quite well after a couple days of a stronger IV antibiotic. “No one was thinking this was anything more than lymphadenitis. We thought we might need it drained or something by an ENT doctor, but we were hoping that was all we were dealing with,” said Neely. Maren was discharged home, as both her team and parents anxiously awaited final biopsy results.
Just 24 hours after returning home, Maren’s energy levels took a big dip. She was also more lethargic, and a second lymph node was now noted in her neck. She returned to SSM Cardinal Glennon where she was admitted to 2 South. Still awaiting biopsy results, an MRI was scheduled for the next day on 10/22. Neely recalls the moment that Maren awakened from that sedated MRI. “The Child Life therapist came in and offered to take Maren out of the room to play. At the same time, this tall doctor with a calm, but serious look on his face came into our room. I asked him if he was the ENT doctor, and I’ll never forget his response,” Neely said. He responded to me in the most empathetic, yet direct way he could, and said, “No – I’m sorry. I’m not ENT. I just reviewed the MRI and preliminary biopsy results. I am afraid to tell you that Maren has cancer.”
Maren was diagnosed with Neuroblastoma. Neuroblastoma is a pediatric cancer that develops from nerve cells in the fetus called neuroblasts. Usually, as a fetus matures and after birth, the neuroblasts develop normally. Sometimes they become cancerous, causing neuroblastoma. Neuroblastoma accounts for 7 – 10 percent of childhood cancers, and each year, approximately 800 new cases are diagnosed in the United States. Treatment depends on the patient’s age and how much the disease has spread.
In Maren’s case, her original tumor was in her abdomen, pushing on her spine. Her MIBG scan showed metastasis of disease to her knees, elbow, skull and bone marrow, classifying her as a Stage IV. Parents Neely and Chris were prepared with a “roadmap” of therapy, which would involve months of chemotherapy, surgery, autologous stem cell transplant, radiation and immunotherapy.
Maren was enrolled in the Neuroblastoma NMTRC012 study. SSM Health Cardinal Glennon Children’s Hospital is one of 53 pediatric centers worldwide that has ability to enroll patients in this study. With parental consent, the study involves sending tissue biopsy samples for genetic testing at time of diagnosis with a goal to determine if there is an additional “targeted therapy” agent – unique to the patient’s genetic tumor markers – which can provide an additional “unique tumor cell attack” to supplement the already “gold standard” of therapy. The tissue samples were sent, and her protocol would adjust accordingly to add additional therapy depending on the results of her genetic testing.
Maren’s first round of chemotherapy started on 10/28. After her second round of chemotherapy, she had a “stem cell apheresis”. This procedure is done in preparation for eventual “autologous” (meaning obtained from the same person) stem cell transplant. In this type of transplant, the patient is both donor and recipient of blood-forming stem cells, which are collected and frozen until needed. In Maren’s case, transplant was planned after her final round of chemo.
Maren completed 5 total rounds of chemo before the surgery to remove her abdominal tumor. An additional targeted therapy agent, Dsatinib, was added to Maren’s regimen in the 3rd cycle based on her tissue sampling sent for genetic testing. Over the course of those months, she lost her hair, experienced a great deal of nausea and vomiting and weight loss. She had a gastrostomy tube placed for enteral feedings between her 3rd and 4th rounds. She also spent her 3rd birthday in the hospital.
Maren’s 10-hour surgery to remove her abdominal tumor took place on February 18, 2020. While the surgery was very successful, the weeks and months to follow brought many challenges including increased vomiting, a second surgery for intussusception (a condition in which one segment of intestine “telescopes” inside of another, causing an intestinal obstruction (blockage), the beginnings of TPN (IV nutrition therapy) at home for continued nutrition support, a final round of chemotherapy, and one more surgery in April for another bowel stricture.
On April 28th, Maren was admitted for her autologous stem cell transplant. She received high-dose chemotherapy first. This destroys any remaining cancer cells in the body, as well as the normal cells in the bone marrow. After high-dose chemotherapy, her previously collected frozen stem cells were thawed and given as a blood transfusion.
The stem cells travel through the bloodstream and settle in the bone marrow. During her recovery and remaining time in the transplant unit, the stem cells begin making new white blood cells, followed by new platelets, and new red blood cells. She was hospitalized for 36 days and was discharged home.
In an AUTO transplant, there is little risk of rejection because the replacement stem cells are the patient’s own cells. However, there is a risk in an autologous transplant that some of the cells that are put back into the patient could still be cancerous. So – Maren’s next treatment would be radiation. The goal of radiation is to destroy any remaining neuroblastoma cells that remain behind after transplant. Maren started radiation treatments on June 17. She finished 12 total rounds of radiation on 7/1.
Neely and Chris received “the best news ever,” as Neely stated, on July 20th. Her MIBG scans and bone marrow biopsy revealed that she was finally IN REMISSION!
The next phase of Maren’s treatment involved the use of immunotherapy. The goal of immunotherapy is to boost the patient’s own immune system with a combination of medications and targeted agents to fight off any remaining cancer cells. Maren completed 6 rounds of a complex rotating schedule that involved week-long hospital stays, injections at home, daily oral medication and more. Her first round of Immunotherapy began 7/26 and her last round finished in December 2020 around her 4th birthday. The plan following immunotherapy was to continue an oral chemotherapy agent for 2 years and have regular MIBG scans to evaluate whether her remission would continue with no evidence of disease. Due to side effects from chemotherapy Maren sustained moderate to severe hearing loss and utilized hearing aids in both ears.
Maren experienced many ongoing clinical challenges in the months ahead, such as continued bowel, vomiting and nutrition issues, she showed her “might” and grit DAILY; however, Maren’s Neuroblastoma returned. Throughout the remaining months of her life, her resilience and that of her parents was noted deeply by her care team. Neely referred to staff of the Costas Center and 4 North as “family.” “They loved Maren, and our other daughter, Mercer, and they cared for us, as parents, too. They took the opportunity to get to know us and continued to do so MORE every time we visited. There were always a lot of special touches, too. We had Easter baskets, Halloween candy and treats, and birthday parties thanks to Justine from Child Life; some much appreciated food delivery from Aleeza in Social Service. The 4 North nursing staff went out of their way to provide Maren with the best care possible. They always provided fun activities and toys to help make the most out of her stays. We had dedicated coordinators like Brittany, Courtney and Sarah anticipating and answering all of our questions and giving us their cell phone numbers. The list goes on. We want to thank all her caregivers including the numerous doctors, nurses and therapists who took fantastic care of Maren,” says Neely.