Our Patients:
Olive Craft

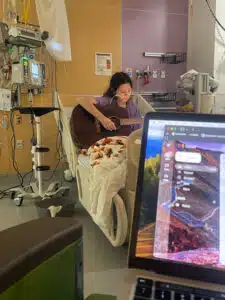
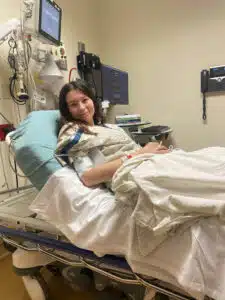
Seventeen-year-old Olive is a stunning young lady. She is a high school junior with a recently acquired driver’s license; a self-taught acoustic guitar player with the world at her feet. Being able to attend school full-time in person, take a trip to Target, and walk the mall – these are the happiest and most “normal” days Olive has seen for as long as she can remember.
Olive’s mom, Suzie, Director of Marketing and Partner- NICHE Food Group in St. Louis, MO, remembers Olive’s early years as anything but “normal”. “Olive was a colicky baby,” Suzie said. “She always needed alone and quiet to fall asleep. She choked a lot when she nursed, and she had awful constipation early on, as an infant. When she began eating table food, she seemed a little happier. She ate everything placed in front of her, until one day, it just suddenly changed. Olive developed these strong aversions to texture and anything that was remotely sour. She wouldn’t eat fruits or vegetables, and she developed rashes with peanuts and tree nuts,” Suzie said. “I was a young mom, and her dad was an accomplished chef. We own multiple restaurants and live our life around food. It seemed ironic that a little girl who had exposure to almost anything a palate could want – could be so incredibly miserable. I put all my energy during those years toward being a mom to her and her older sister. I felt like a failure, and no one really had answers”.
From the time Olive was a toddler through her early elementary school years, Olive continued to have food aversions and ate very little amounts of food. “Her doctors felt she would grow out of it,” said Suzie. “She was able to meet adequate milestones for her weight, and aside from also being diagnosed with asthma, there wasn’t anything alarming which made them want to test her for anything further. She was a great student, and was involved in all kinds of extracurriculars, clubs and camps. She danced 5 days per week at St. Louis Academy of Dance. It wasn’t until the middle of elementary school that we had a few more reasons to be concerned.”
Around third or fourth grade, Olive had repeated visits to the orthopedic injury clinic. Her “picky eating” escalated, eventually being diagnosed with ARFID (Avoidant/Restrictive Food Intake Disorder) an eating disturbance characterized by restricted food intake that isn’t caused by a distorted self-image or a desire to change your weight. Rather, it’s a result of anxiety or phobia of food and/or eating, a heightened sensitivity to sensory aspects of food such as texture, taste or smell, or a lack of interest in food/eating secondary to low appetite. “Olive had a fear of vomiting. Her anxiety was so bad. She would have panic attacks about her health, which made it even more complicated for doctors to evaluate her,” Suzie said.
Both Olive AND her older sister, Ellie, seemed to always be getting injured and had several occurrences of broken ankles and bones. Doctors referred to them as “bendy”; however, offered no explanation of why they were repeatedly getting hurt. “In the 6th grade, Ellie grew more and more frustrated each time she got injured. She googled her symptoms, and she found a condition called Ehlers-Danlos syndrome (EDS),” Suzie said.
Hypermobility or a flexible “bendy” body is a hallmark of some types of EDS. EDS is a group of genetic disorders that make your connective tissues weaker and more flexible than normal. Ehlers-Danlos syndrome can affect any connective tissue in your body (including your cartilage, bones, blood, fat). Depending on where EDS affects your connective tissue, your symptoms can show up differently. Most people with Ehlers-Danlos syndrome don’t know they have a genetic mutation, so doctors usually diagnose it based on a patient’s symptoms and medical history. EDS can be inherited from a parent with the same faulty gene or alternatively, someone can be born with a new mutation so that the condition is occurring in their family for the first time.
Suzie took both Ellie and Olive to a geneticist. Getting a diagnosis involves looking for joint hypermobility, signs of faulty connective tissue throughout the body, a family history of the condition, musculoskeletal problems (i.e. long-term pain, dislocations), and a host of other criteria. Both Ellie and Olive received a confirmative diagnosis of EDS. There is a whole spectrum of EDS types, the most severe form of which (vascular EDS) can lead to fatal complications like arterial, intestinal or uterine ruptures. In many cases, people with vEDS are identified only after a severe complication or death. Confirmation of vEDS requires genetic testing to identify pathogenic mutations in a particular gene.
Both girls underwent genetic testing, echocardiograms and cardiology consultation. Ellie was discovered to have both a bicuspid valve and aortic aneurysm and continues to be followed by a cardiologist, but neither tested positive at that time for the vascular type of EDS. Suzie’s next focus was what she and the girls needed to do for their ongoing health maintenance. Both Ellie and Olive had continued GI issues, routinely didn’t feel well, and were tired of getting hurt all the time. “I was told that there was really nothing to ‘DO’ – that lots of people with EDS have GI issues and to have them work on strengthening exercises,” said Suzie.
“There are so many associated symptoms and disorders with EDS which are not part of formal diagnosis criteria, and not a result of ‘bendy joints’,” Suzie said. “Some people have orthostatic blood pressure issues, digestive disorders, and anxiety disorders. These can even be worse for quality of life than the joint symptoms people present with.”
“Both my girls had so many GI issues. Both of my girls, also, established regular routine visits with a psychiatrist. Similar to Olive, Ellie had multiple GI consults, allergy consults and more. She was diagnosed with SIBO (small intestine bacterial overgrowth), which spiraled into an eating disorder. She developed severe anorexia and was treated at a residential treatment center in Chicago for several months,” Suzie said.
As Olive grew older, she wanted to go away to boarding school. Despite her ongoing ARFID and GI issues, she managed to keep dancing 5 days/ week and keep up with her studies and pace at school. She did notice, however, that during her periods, she would lose a lot of blood – leading to instances of dizziness and fainting. Her eating became less and less, and she would feel really full after eating just a few bites. When she returned home for spring break in 2024, she was clearly malnourished and had difficulty standing. Suzie took her to a hematologist, who mentioned Olive might have POTS. Postural orthostatic tachycardia syndrome (POTS) is a condition that causes a number of symptoms when you switch from lying down to standing up, such as a fast heart rate, dizziness and fatigue. Normally, your body’s nervous system balances your heart rate and blood pressure to keep your blood flowing at a healthy pace, no matter what position your body is in. If you have POTS, your body can’t coordinate that balancing act of blood vessel squeezing and heart rate response. So if your body can’t keep your blood pressure steady and stable, this causes a variety of symptoms like dizziness, fainting and exhaustion. During her visit to the hematologist, Olive could barely stand without help. She had an iron infusion and some IV fluids and they encouraged her to increase both her salt and her water intake. She would return to the hospital with follow-ups to both the GI clinic and POTS clinic. Over the next couple months, Olive’s malnutrition escalated and she got to the point where she couldn’t even drink water. She was admitted to the hospital for just a little over a month. As a starting point, Olive had a feeding tube placed. And though motility issues were a possible culprit, the hospital did not have motility testing available. Her ARFID and accompanying anxiety earned her the label of having an eating disorder and by the end of her one month stay, her adolescent medicine team recommended residential care for just that.
“I didn’t feel supported or listened to,” said Suzie. “I felt like because Olive’s older sister had an eating disorder, her doctors were convinced Olive’s issues were solely in her head. We followed through as instructed and took Olive to the same inpatient facility in Chicago that Ellie had been treated at. That was in November of 2024. I knew there was something we were missing. I just didn’t know what,” said Suzie.
Olive had only been in Chicago for 2-3 days, when Suzie received a call from the physician in charge of her care. “He told me he thought Olive would do better at home,” Suzie said. “I brought her home, chose not to work and fully dedicate my time to finding out how to help her. Over the next several months, I made calls to Johns Hopkins, Mayo Clinic, Cleveland Clinic, CHOP, Boston Children’s…. multiple places, to see if anyone had a program or a person that could take a more comprehensive look at my daughter. At the beginning of January 2025, I received a call from CHOP which has a Center for Amplified Musculoskeletal Pain Syndrome (AMPS) which focuses on chronic pain conditions and provides a comprehensive Lifestyle Medicine Program for connective tissue disorders. Olive Met the criteria to be seen by CHOP’s multidisciplinary GI clinic, and we secured an appointment. As we awaited that date, which was several months away, Olive’s psychiatrist encouraged us to do some research on dysautonomia specialists in the area, ideally a neurologist. The first practitioner I found was Dr. Laurence Kinsella, who is an adult dysautonomia specialist with SSM Health. I asked his office for a recommendation to a pediatric dysautonomia specialist, and they recommended Dr. Cynthia Morris, a neurologist and dysautonomia specialist at SSM Health Cardinal Glennon. Olive had never regained her strength. She continued to suffer with all of her same symptoms, and at this point, had been in a wheelchair for several months.”
Dysautonomia refers to a group of disorders that affect the autonomic nervous system (ANS). The ANS is part of the nervous system. “Autonomic” means “self-governing,” and the ANS manages the body system processes you don’t think about (things like blood pressure, body temperature, breathing, digestion, heart rate, sweating and more). If you have dysautonomia, one or more of those ANS processes aren’t working as they should and your symptoms could include anything from lightheadedness or fainting when standing up, rapid heart rate, low blood pressure, dizziness, fatigue, sweating abnormalities, digestive problems or urinary problems.
“Dr. Morris is the only pediatric dysautonomia specialist in Missouri, so I was concerned about being able to get an appointment. We were able to get in right away, though, on January 9, and our visit with her was outstanding, to say the least,” Suzie said. “Olive felt validated and heard. She acknowledged that abdominal pain in EDS can be a puzzle with countless hidden pieces…. that there are surprising connections between the spine, bladder, ribs, gut and brain, that can explain symptoms often dismissed or misunderstood,” Suzie said. “Along with some other suggestions, she referred Olive to pediatric gastroenterologist, Dr. Aniruddh Setya and strongly recommended she be evaluated in his IMAGINE clinic.
The IMAGINE program (Integrative Medicine Addressing Gastrointestinal Needs with Evidence) at SSM Health Cardinal Glennon helps children struggling with digestive challenges by providing them with holistic, evidence-based care that treats the whole person, not just the symptoms. The goal of the program is to combine the best of modern medicine with complementary and integrative therapies to help children with digestive challenges thrive. The multidisciplinary team includes a gastroenterologist, a child psychologist, and a social worker and dietician. What makes the IMAGINE program distinct in the region is its specific, holistic approach to treating pediatric digestive problems
“We saw Dr. Setya and his team in early February. Our appointment was incredible. They took so much time with us gathering Olive’s history and really getting to know her. They also told me Cardinal Glennon has a specialized GI motility clinic. It was surprising and so reassuring to me that we could have such a comprehensive evaluation done right here in St. Louis, and I had no idea,” Suzie said.
Several recommendations from the IMAGINE team came out of that visit. Olive started a few new medications and supplements to address her stomach spasms, nausea and constipation. She incorporated aromatherapy, began a gastroparesis diet and started weekly acupuncture, which stimulates her nervous system, just to name a few. “She was given the tools to manage herself,” Suzie said. “They believed in her and trusted her and she was willing to try ANYTHING,” Suzie said.
By the time Olive had her next appointment with her adolescent medicine doctor, she had started gaining weight. She noticed subtle improvements from many of the holistic therapies and supplements and was able to go without her wheelchair, which she hadn’t been able to do in months. “We followed up with Dr. Setya at the end of February and she was doing so much better that he told Olive she could just see him as needed,” Suzie said. “Spring and summer were all about rebuilding because she was so de-conditioned from being sick,” Suzie said. “She’s been taking activities slow, continues her gastroparesis diet, her weekly acupuncture which she has really come to love, and her regular visits with her psychiatrist. She began online summer classes for school during the summer, returned to school full time as a junior this fall, and has even gotten her drivers’ license, which was such a huge milestone for her.”
“I truly can’t say enough about what we’ve found in SSM Health Cardinal Glennon. We continue to see Dr. Morris and we have transferred her adolescent medicine care to Glennon, which has been life-changing, as well. Dr. Libby Noonan and Dr. Muir have truly seen and validated Olive and we are taking life one day at a time. The IMAGINE clinic gave Olive sustainable changes – which empowered her to become an active participant in her own health journey. I only wish we had known about all the services here sooner, and I am proud to share our story if it can empower any other family the way Cardinal Glennon has mine.