Our Patients:
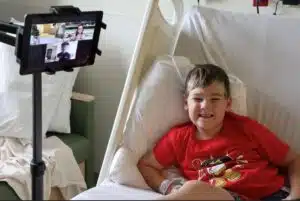
Ryder Lee

Ryder became a patient at SSM Health Cardinal Glennon long before he was even born.
The long-anticipated son and 4th child of parents Sarah and Nathan, Ryder has successfully won the hearts of his 3 older sisters and his second family here at the hospital.
Sarah recalls the trip to her obstetrician for her 19 week ultrasound. She was anxiously anticipating to find out if her 4th child was going to be a boy. She got the news she wanted! God has blessed her with a boy! But she also heard additional news that no one can ever truly prepare you for. The OB found fluid on the baby’s brain during that scan, so he promptly referred Sarah to see a maternal fetal medicine specialist. More brain and spinal images were captured on ultrasound, and the MFM found what he thought to be spina bifida. “He was spewing out all sorts of terms that I had never heard of. He encouraged me NOT to Google,” Sarah said, “but to make an appointment with the Fetal Care Institute at Cardinal Glennon.”
Spina bifida is a birth defect in which an area of the spinal column doesn’t form properly. This leaves a section of the spinal cord and spinal nerves exposed through an opening in the back. Spina bifida is the most common central nervous system birth defect, and it occurs in approximately 1 per every 2,000 live births in the United States. The most common and serious form of spina bifida is called myelomeningocele (MMC), in which part of the spinal cord and surrounding nerves push through the open bones (vertebrae) in the spine and protrude from the fetus’ back. The myelomeningocele lesion can occur at any level on the developing spine, but most are found in the lumbar-sacral region. Depending on the lesion’s location, myelomeningocele may cause: bladder and bowel problems (incontinence), weakness and loss of sensation below the defect, inability to move the lower legs (paralysis) and other cognitive impairments, sexual dysfunction, and/or orthopedic malformations such as club feet or problems of the knees or hips. Generally, the higher the defect is located on the spine, the more severe the complications. In many cases of spina bifida, the brain develops what’s called an Arnold-Chiari II malformation, in which the hindbrain herniates or descends into the upper portion of the spinal canal in the neck. This herniation of the hindbrain blocks the circulation of cerebrospinal fluid, causing hydrocephalus (accumulation of fluid in the brain), which can injure the developing brain. Ventricular shunting (placement of a thin tube into the ventricles of the brain) is used if necessary, in order to drain fluid and relieve hydrocephalus.
At 20 weeks pregnant, Sarah had her appointment at the St. Louis Fetal Care Institute. “It was a lot of information, hard to digest, and very emotional,” said Sarah. “But they gave me what I needed to hear that day – a confirmation of the diagnosis, and the choices and options we had to consider as his parents.”
“We met with the lead neurosurgeon and MFM. We were given the option of putting off the surgical repair until after Ryder was born, or having them perform fetal surgery BEFORE he was born. Both carried a lot of risks and benefits and we didn’t have a lot of time to decide. If we went with fetal surgery, we needed to commit soon. There were risks of premature labor, and possibly even death, but the opening in Ryder’s spine was really large,” said Sarah. For children with spina bifida, the exposed spinal cord and nerves are usually contained in a sac that is exposed to amniotic fluid. The “continuous bathing” of the fragile developing spinal cord in amniotic fluid over the course of gestation is thought to result in progressive neurologic injury.
“We chose to have the fetal surgery,” said Sarah, “and we scheduled it right at 24 weeks pregnancy. I had my surgery at SSM Health St. Mary’s and we were blessed to have everything go smoothly. They were able to close his back, put him back inside me, close me back up, and allow me to recover. I went home within 5 days, and followed up with the FCI 2 times weekly f or the next several weeks,” said Sarah.
At 36 weeks, Sarah began having contractions. She was happy to have an appointment already scheduled for her 36 week check-up. “My OB told me – ‘you’re going to have this baby this afternoon,” said Sarah, and immediately following the appointment, I found myself headed back to St. Mary’s.”
Ryder was delivered via C-section and came out strong and screaming. Overall he appeared healthy, but it was a bit early to tell. His left leg was strong. His right leg was floppy. The fluid buildup to his head was minimal, and he had no breathing issues. His first day went pretty smoothly, but on day 2 he required some oxygen. He was transported to SSM Health Cardinal Glennon via ambulance by the transport team, and admitted to the Neonatal Intensive Care Unit. His first week went relatively smoothly, but then one thing led to another. He failed his car seat test, he began having bradycardia episodes (low heart rate) with increased frequency, and his head circumference measurements were increasing. These were signs of increased intracranial pressure, and the team decided to place a VP (ventriculoperitoneal) shunt in Ryder. He was 17 days old. A few days later, Ryder was much better, and he was stable and ready for discharge.
“It was a little bit scary to go home,” Sarah recalled. “He seemed pretty normal, but we knew we had a lot to watch for, including seizures, developmental delays, signs of his shunt malfunctioning, and more,” Sarah said. “We knew we had resources. It was just hard to not know when and where our challenges would pop up,” said Sarah.
Sarah had contacted Missouri First Steps before birth. Having that in place with weekly visits was comforting once Ryder was discharged. Physical therapy started within one week of him being home, and a dietician was added fairly soon because Ryder was a slow grower. At first, Ryder returned monthly to the hospital to see Neurosurgery, Urology, Orthopedics. At 6 months of age, those visits became less frequent, and his visits became managed through the Spina Bifida Clinic. “Spina Bifida Clinic is amazing. It’s like one-stop-shopping for Ryder’s specialists and needs.” “Anne and Lou are amazing,” says Sarah. “Anne is the Neurosurgery Nurse Practitioner, and Lou is the Nurse Navigator for Urology and Spina Bifida. They’ve walked me through so much from infections to equipment issues to bowel and bladder regimens, multiple surgeries, coordination with Ryder’s specialists and more,” says Sarah.
Since his first year of life, Ryder has had multiple surgeries and procedures to address leg length disparities, bowel and bladder issues, brittle bones and more. He started having seizures at the age of 2, and though medication has helped manage the frequency, he still has them at least once monthly.
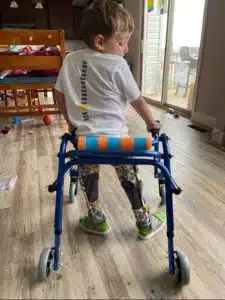
Ryder started preschool at age 3, and loves to stay busy between his dump trucks, toys and his sisters. Not much stops him between his wheelchair and his walker!
“Glennon is really like a second home to us since we spend so much time here,” says Sarah. “When I speak with other parents who take their children elsewhere, they tell me they have a hard time finding doctors who listen to them. I have never had that experience here. Ryder’s doctors listen to me, and I feel like we’re partners in his care. Some of our challenges and conversations are tough. We don’t necessarily always see eye to eye, and we will keep having new sets of circumstances and challenges as he grows and gets older. We started coming here through the St. Louis Fetal Care Institute before Ryder was even born. That was a very sensitive time. They held my hand and brought positivity to a time that we really needed guidance as a family. It’s continued to be a good team as we work together to manage Ryder’s care. We can’t imagine not having our Glennon family,” says Sarah