Our Patients:
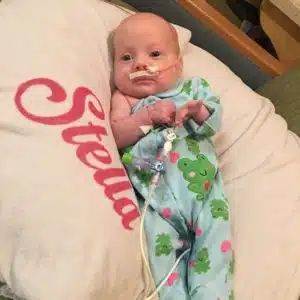
Stella Thomas
Just keep swimming.
If you are familiar with the Disney movie, “Finding Nemo”, you might remember that Dory is trying to find her parents. Through adversity, adventure, uncertainty, and doom she searches and searches. Just when all hope is lost, a light shines on everything and Dory and her parents are reunited. Throughout this movie, Dory has a phrase that she uses to motivate herself in times of trouble: Just keep swimming.
“When the odds were against her, when her parents were lost and confused, when any number of things could have held her back, she just kept going. Just keep swimming is STILL Stella’s theme song,” says Rachael Thomas, mother of this sassy 5-year-old NICU graduate.
At 20 weeks gestation, Rachael Thomas of Farmington, MO was having an uneventful and uncomplicated pregnancy. At her routine, scheduled ultrasound, it was discovered that she had a 50% placental abruption. Placental abruption is a complication of pregnancy that happens when the placenta detaches partially or completely from the womb (uterus) before delivery. This can deprive the baby of oxygen and nutrients. Placental abruption is related to about 1 in 10 premature births (10 percent).
Premature babies (born before 37 weeks of pregnancy) are more likely than babies born later to have health problems during the first weeks of life. Rachael was monitored closely over the next several weeks. She was placed on bedrest, and prepared for a possible early delivery.
“I was 28 weeks and stared having strong and frequent contractions. They admitted me to the hospital for Magnesium to slow my contractions down, but my sassy girl apparently had other plans!” Rachael said. “Stella made her entrance into the world, and ready or not, we were on a trip that no parent is really ever prepared for.”
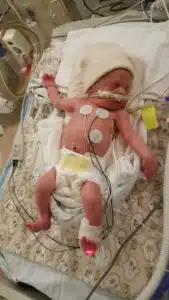
“I remember waiting for her to cry. We breathed a sigh of relief once we heard her, but then the doctors and nurses swept her away to another room. We weren’t sure when we would see her next or if we’d even get to hold her,” said Rachael. “They brought her back in the room in what looked like a microwave to me! I know now that it was a transport incubator, but at the time, it just looked so scary. My husband and I were able to touch her before she left, and then we watched her and the helicopter fly away.”
Stella was airlifted to SSM Health Cardinal Glennon Children’s Hospital in the safe care of the neonatal transport team. She arrived to the Dana Brown Neonatal Intensive Care Unit (NICU) for what would be a 180 day adventure.
“As hard as it was to watch her go, we knew she was going to the right place. We were also given a little evidence of her willingness to fight. Apparently when they tried to put her breathing tube in, she fought it so hard that the anesthesiologist was called to do it.
She fought back so hard during his attempt that he decided she was strong enough to breathe on her own and that she was safe for transport without it. He intentionally stopped back in our room to tell us we had a fighter on our hands,” Rachael said. “You have a fierce little girl in Stella,” he said.
Just keep swimming. Be ok being uncomfortable.
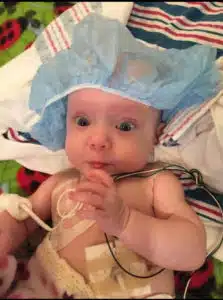
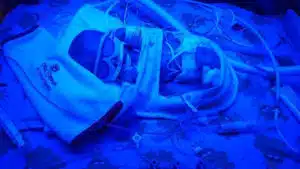
“Sometimes persevering means that we have to do things we don’t like. We knew we might have to make hard decisions, do things we’re not good at, or any number of countless things,” said Rachael. Adjustment to NICU life was overwhelming We really couldn’t hold or touch her much in the beginning. She was in a Giraffe bed under bilirubin lights, and had CPAP (continuous positive airway pressure) to help her breathing. There were turning routines, skin care routines, IV’s and so many things to learn about our girl,” said Rachael.
The Giraffe Omnibed is a state-of the-art piece of equipment which provides premature and ill babies with a controlled, stress-reduced environment, much like that of a mother’s womb. It helps regulate body temperature and features humidity control to avoid moisture loss through thin skin. The NICU is able to purchase and update these beds as needed through generous donor support to SSM Cardinal Glennon Children’s Foundation.
Surprisingly after 3 short weeks, Stella transitioned to the infant unit on 2 South. She was bottle feeding and the team felt she could safely grow and gain weight outside of the NICU environment. Unfortunately, just as quickly as she left, she returned to the NICU for vomiting and belly distention. Stella’s abdomen distended to three times its normal size, and she was no longer tolerating her feedings. The next several months were a storm that included daily x-rays, upper and lower GI’s, biopsies of her intestines, tons of replaced IV’s and feeding tubes and so much more. She was tested for many different conditions including hirschprung’s disease and cystic fibrosis, but all tests came back inconclusive.
Just keep swimming. Don’t go alone.
“Seeing her vomit so much and constantly pulling out her tubes – it was so frustrating not to have a diagnosis and a reason. But despite all of it, the doctors and nurses were AMAZING and that NICU was our home away from home. We were able to choose a primary doctor and primary nurses and the private rooms were just as big of a blessing,” said Rachael. “I honestly can’t imagine what parents would do without private rooms,” says Bobby, Stella’s father. “Parents go through everything there. There’s a lot of teaching and learning going on. There’s a parent next door celebrating and a parent in the next room grieving. I can’t imagine having to go through the spectrum of what you go through during all that time, in a shared space. And having primary nurses built our confidence to go home as we needed. We had two other daughters and two full-time jobs. Trying to keep it all afloat meant being able to trust Stella’s care team,” Bobby said.
“They saw our concerns, and were willing to have many difficult conversations with us,” says Rachael. “They always had Stella’s best interests at heart and encouraged the path that would make Stella her most viable self – not the path that would make us the most happy as parents. Those crucial conversations helped us understand that anytime we left, we could trust their care of her. Even aside from her primary care team, the whole hospital treated us like family. From the Child Life therapists to the housekeepers, the café staff to the front desk greeters, everyone knew us and helped us feel comfortable. We had all the specialists we needed for HER right at our fingertips, plus social workers, and things like the Ronald McDonald House Family Room which helped us as parents,” Rachael says. “Stella’s sister, Fiona is currently 12, but she was 6 years old when Stella was born. “I remember Nurse Helen and the Child Life therapist taking an interest in me and helping me out whenever I visited my sister,” Fiona says. “I was six, so I couldn’t really put words to how I felt. They could sense when I was upset or concerned, and they made time to talk with me or occupy me with things to do while I was there. They always allowed me time and opportunity to talk about how I felt or what was going on with ME. They made the hospital a safe place for me, and made me feel less scared about things,” says Fiona.
Just keep swimming. Keep your eye on the prize.
From September, when Stella returned to the NICU, through December of 2016 when they were discharged home, there were many ups and downs. For the better part of September, Stella was not eating well. She was losing weight and she was lethargic. She needed a central line placed due to multiple failed attempts at accessing her peripheral veins. She also needed a gastrostomy tube placed for consistent nutrition. Occupational therapy, physical therapy and several other evaluations and tests revealed proper brain waves and brain wave activity, which gave Rachael and Bobby hope that Stella could “fight” whatever this condition was. All suspected diagnoses had been ruled out. There was still no “name” or explanation for her symptoms. “Her symptoms were most similar to a condition called megacolon. She just needed to grow into her bowel and that would take time. The goals were to keep her nutritionally balanced, maintain her weight and get her home. We would be going home with feeding pump and on a short leash with her doctors and dietician, but we were just as determined as Stella was to finally get home,” says Rachael.
Over the next few months and trials of multiple dietary formulas and regimens, the Thomas family got their wish. Stella was discharged home just before Christmas in December, 2016. “We had reevaluated the course we were taking with Stella multiple times. But her team never stopped going, and they fought for solutions as hard as she fought through everything. Everything her doctors researched and everything they tried brought us one step closer to us going home as a family,” says Rachael.
“After we got home, I think I called our dietician, Chelsea, every day,” recalls Rachael. “In fact, I probably texted or called her multiple times each day!. She tweaked and adjusted the meal plan for Stella constantly based on her weight and observations I would jot down about Stella in my journal.
Our daily lives and environment went through a lot of change, too. I quit my job to care for Stella full time, and our kitchen looked like a hospital room,” Rachael laughed. “She had regular occupational therapy and physical therapy, tummy time and developmental exercises to work through each day. She also had weekly home nursing checks and at LEAST daily check-ins with her dietician. We converted some of our cubbies into supply organizers for all of Stella’s syringes and tubes. We even had to buy a mobile like the one she had in her NICU room because that particular mobile was one the only things that soothed her. After several sleepless nights together, and a social visit back to the NICU where she acted more calm and at peace than the whole time we had been home, we realized that NICU had really become her primary “home”. Adjusting to her new home with us would take some time,” acknowledged Rachael. “We returned for clinic visits every 6-8 weeks and gradually evolved the first year from a continuous daily tube feeding to 8 intermittent feedings each day. This gave both Stella and us a little more freedom and by the next year, we had adjusted to only 4 feedings per day. Around her first birthday, Stella was la grazing and experimenting with table foods. It was mostly puree-like foods such as oatmeal, rice cereal and baby food, but she was open to it. We looked forward to the day when she could both feel and satisfy hunger signals with real food, and when she could sustain her weight and nutrition without the need for pumps and formula,” Rachael says.
“I logged everything in Stella’s food diary every day for those first two years. With time, her table food intake increased, and her need for formula was able to decrease. Then one day, on July 4, 2018, she dislodged her feeding tube in the back of the car, and we had formula spill over the entire back seat. That day I decided there was no going back. This was an opportunity for us to gauge if she was physically and mentally ready to be done with her pump. As soon as we got home, I gave her a cup. She figured out when she was hungry, and the rest is history,” Rachael says.
“Weeks later, Stella and I took the pump to the UPS store to send it back to the rental company,” Rachael says. “When we got in the car to go home, she told me she wanted it back. I realized that pump had been like a best friend to her for two years. It kept her alive. It soothed her to sleep. Life without it would bring so much more independence, but it was also so much of what she knew to be normal,” says Rachael.
Still swimming….
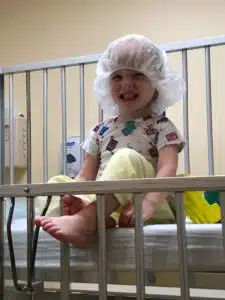
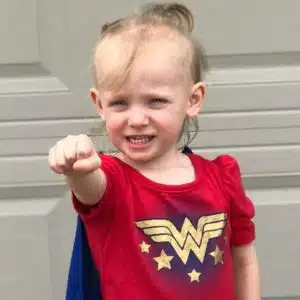
Stella had surgery to remove her gastrostomy button in December 2018. “Today, she eats like a horse,” Bobby says. “Her favorite foods are strawberries, broccoli, peppers, Little Debbie Snack cakes and Lunchables,” he says. “She’s a sassy bucket of joy and loves gymnastics, being outside, anything that involves creating and building, and anything that involves climbing. She climbs rock walls, cabinets, and scales walls with no fear. To watch her do cartwheels and all of her gymnastic moves, you would never know from her mindset or actions that she had such a fragile beginning,” Bobby says.
“Bobby and I simply don’t have enough words or actions to show the gratitude and appreciation we have for SSM Health Cardinal Glennon,” says Rachael. “We seek ANY opportunity to share our praise for the hospital and all of the people that work there. When you find a treasure, you just want to share it with anyone who will listen. We can never repay what was given to our daughter. Hopefully sharing our story is just a small way to pay it forward.”