Our Patients:
Wyatt Beckett
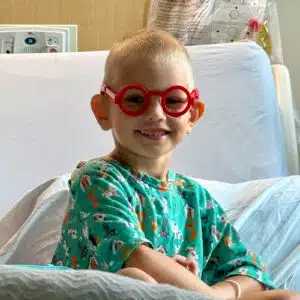
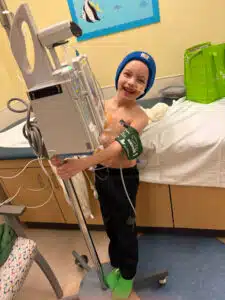
Before hospitals, transfusions, or isolation ever entered his world, Wyatt was simply Wyatt: an active, unstoppable 3‑year‑old growing up on a busy farm almost two hours southeast of SSM Health Cardinal Glennon Children’s Hospital. His days were spent riding tractors, chasing goats and donkeys, helping bale hay, and exploring acres of open land with his big brother, Stetson. Indoors, he loved Paw Patrol and Blaze and the Monster Machines. “He’s all boy,” his mom Heather says. Life was wide‑open, loud, and free—long before anyone realized something was quietly wrong.
Looking back, Heather remembers small clues sprinkled across several months. In April/May 2025, Wyatt hit his head at a baseball game and developed a large bruise. The ER ruled out a skull fracture and recommended a follow‑up visit with their pediatrician one week later. Around the same time, multiple extended family members had mentioned Wyatt looked “yellow.” Heather took advantage of timing and asked at Wyatt’s follow-up visit if there should be cause for concern. The pediatrician was not fazed by Wyatt’s coloring or presentation and dismissed Heather’s request for lab work.
By August, Wyatt was sleeping more, tiring easily, and bruising frequently. His constant activity made these changes easy to excuse—until a cousin cutting his hair mentioned he looked pale and worn out. That comment pushed Heather to send a MyChart message to his pediatrician asking once again for labs. This time, the lab work was ordered, and Heather took Wyatt to a nearby office that afternoon.
Later that night, everything changed. The pediatrician called Heather and husband, Tyler, with results too urgent to wait: Wyatt’s blood counts were dangerously low. He instructed the family to proceed immediately to the nearest emergency department. In shock, Heather and Tyler did just that, while Stetson stayed with grandparents. Wyatt’s platelet count was 5; his hemoglobin was 3.5. Transfusions were started immediately, and knowing he would need care at a pediatric tertiary care center, the care team from the local hospital called the ACCESS Center at SSM Health Cardinal Glennon. An emergency transfer was recommended, a helicopter was deployed for transport, and Heather, terrified yet determined, advocated flying with him. Though every circumstance is different, Heather was allowed to fly with Wyatt in the helicopter. Tyler drove separately and would meet up with them as soon as he could.
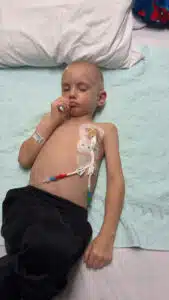
After arriving at Cardinal Glennon in the wee hours of the morning, Wyatt was quickly admitted to 4 North – the impatient hematology/oncology unit. Heather met a steady stream of providers the next morning and one stood out the most: Dr. Christopher Hugge, the attending hematologist/oncologist. He explained that Wyatt’s symptoms suggested either leukemia or aplastic anemia. A bone marrow biopsy was needed to confirm which condition Wyatt had. He had that biopsy and a PICC line (peripherally inserted central catheter) placed later that day.
Within 24 hours, the diagnosis was confirmed. Wyatt had aplastic anemia, a rare condition where the bone marrow fails to produce enough new blood cells (red, white, and platelets), leading to severe fatigue, infections, and bleeding. Aplastic anemia can occur at any age. It’s usually caused by autoimmune attacks on stem cells, but can also stem from toxins, viruses, or genetic factors. Treatments include blood transfusions, medication, or bone marrow transplants, offering a variable, sometimes curable, prognosis depending on severity.
Wyatt started on anti-viral and anti-fungal medications due to his susceptibility to infections. He was also started on Promacta to stimulate his bone marrow cells to produce more platelets and reduce his risk of bleeding. He remained in the hospital for the next few days and both Tyler and Heather were given a crash course in how to care for his central line, give him his medications and monitor him for signs and symptoms of infection.
After discharge, the family traveled to The Costas Center twice weekly for labs, transfusions, and discussions about future treatment. Both Wyatt’s parents and his care team felt that a bone marrow transplant would be Wyatt’s best chance at a cure. Usually, siblings provide the best match in a transplant scenario; however, Wyatt’s brother Stetson was tested and found NOT to be a match. Twice weekly visits to Costas continued over the next month and eventually in October, a perfect 10 out of 10 match was found in Germany through the National Bone Marrow Donor Registry. A 10 out of 10 match, or 10/10 HLA match, means the donor and recipient have identical human leukocyte antigen (HLA) proteins on their cells, representing a 100% match. This is the ideal scenario for a bone marrow transplant, significantly reducing risks of graft-versus-host disease (GVHD) and transplant rejection, leading to better survival rates.
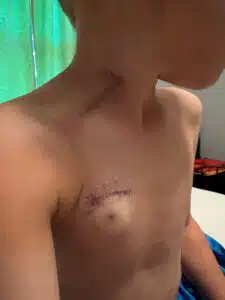
Wyatt had a port placed and continued regular transfusions. On November 17, Wyatt was admitted to the transplant unit on 4 North. “Our donor was traveling after the holidays, so we had to move forward,” Heather said. “If losing one year of holidays meant giving Wyatt many more healthy ones, it was worth every moment.”
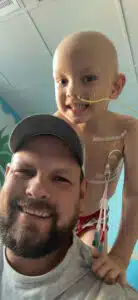
Another central line was placed, and he began five days of intense chemotherapy to clear out diseased marrow and prepare his body to accept the donor cells. He tolerated treatment better than many children but still required a nasogastric tube for nutrition and medication. Transplant Day came on November 26—the day before Thanksgiving.
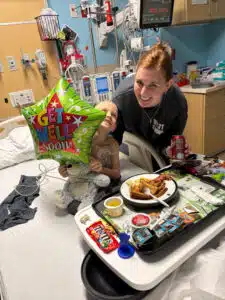
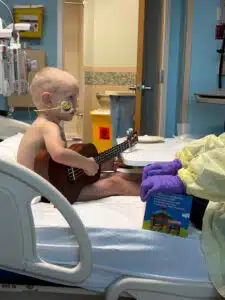
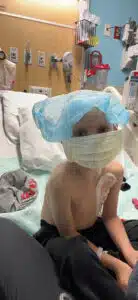
The family spent Thanksgiving, Christmas, and New Year’s in transplant isolation. Heather had 12 weeks of FMLA from her job. She only returned home twice for quick visits with her other son throughout the course of the 50-day stay. She discovered her own strength and voice and appreciated the kindness, compassion and empathy of the staff throughout the process. “He had so many big emotions to let out and had nowhere to go with them. I couldn’t expect him to understand all the restrictions and procedures. Not one part of transplant was what someone his age would ever understand. He was so used to having acres of ground to play on and be able to explore, play and express his feelings through physical activity, around animals, with his brother. We had 4 walls and just each other. No visitors. No escapes. Managing feelings and finding ways to stay uplifted and busy became our everyday job. The Child Life Specialists and Music Therapists tried hard to supply him with outlets. They gave him things like a punching bag, kinetic sand, and tons of coloring supplies. They brought him a drum set, a ukelele, and encouraged me to take breaks when they were able to visit with him, so that I could have even just a few minutes of respite time myself.
The cells received on transplant day move through the bloodstream and into the bone marrow and when the cells begin to grow and create new blood cells, it’s called engraftment – which is an important milestone in recovery. Wyatt engrafted 14 days after transplant. Engraftment means your new cells are working properly and are starting to rebuild your immune system. White blood cells are the first cells to engraft, followed by red blood cells and platelets. For Wyatt to be discharged, he would need his blood counts to continue to rise, be eating well and have no evidence of Graft Vs. Host Disease (GVHD).
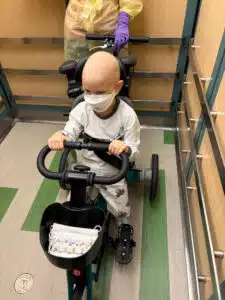
Wyatt was discharged from the hospital on January 6, 2026. Wyatt and Heather stayed at the local Ronald McDonald House for the next month to be close to the hospital for check-ups. Ten days into their stay at Ronald McDonald House, Wyatt was finally able to see and actually touch his brother. “It was an incredibly emotional moment for the whole family with all four of us able to spend a night together,” Heather said. He had outpatient visits at The Costas Center three days per week for the first month. Those visits eventually spread out to twice weekly and are currently once weekly unless otherwise needed. He was able to get rid of his nasogastric tube quickly after discharge. His appetite and energy are high, and he remains on several medications to ward off infections and GVHD. Though his visits to the hospital have decreased, Wyatt is still heavily restricted. He cannot go “out” or go anywhere outside his home environment such as to school, church or stores/restaurants. He is isolated from friends/extended family and can’t be around most animals in an inside environment.
“I can’t wait for the day he has fewer restrictions and can be around other kids again,” Heather says. “I’m so grateful to the nurses and staff at the hospital. A pediatric hospital is SO different from a community hospital. They understood and taught me everything I needed to know as Wyatt’s mom to be able to navigate this journey and continue to advocate for him. They understood the struggles, offered their support, and did everything they COULD do to make the difficult times less challenging. Looking back, I wish I had been more persistent in getting lab work done sooner. The things I never wanted to know have definitely made me a stronger mom and advocate for my child. I encourage every mom I encounter now to follow their gut instinct and utilize the excellent resources in the community to get the best care for your child.”